THE ROLE OF HERBAL COMPOUNDS IN THE TREATMENT OF CEREBRAL ISCHEMIA
HTML Full TextTHE ROLE OF HERBAL COMPOUNDS IN THE TREATMENT OF CEREBRAL ISCHEMIA
Seyyed Hossein Hassanpour * 1 and Seyyedeh Zeinab Karami 2
Young Researchers and Elite Club 1, Yasooj Branch, Islamic Azad University, Yasooj, Iran.
Department of Biology 2, Faculty of Basic Sciences, Yasouj University, Yasouj, Iran.
ABSTRACT: Stroke is the sudden blockage or rupture of cerebral arteries that can lead to cerebral damage or clinical neurologic deficit. Generally, stroke is as ischemic and hemorrhagic. Ischemia caused by factors such as thrombosis, embolism, and systemic hypoperfusion. Stroke is one of the most important factors of mortality and disability worldwide. After a stroke, an increase of free radicals has the most important role in the breakdown of blood-brain and increase of cerebral edema. This study aimed to review the effect of compounds isolated from plants to reduce cerebral ischemia. Our review showed that natural compounds could exert a protective effect by reduction of oxidative stress and events related to it. We also suggest that consider special attention to natural product for the treatment of cerebral ischemia.
| Keywords: |
Stroke, Cerebral ischemia, Oxidative stress, Natural product
INTRODUCTION: As defined by the World Health Organization (WHO), stroke is the rapid loss of brain function during the impairment of brain perfusion 1. Stroke is the main cause of mortality and disability and commonly occurs during the elderly so that it burdens high expenditure to health field to the reduction of complications related to stroke 2. These patients are prone to other problems such as pneumonia and urinary tract infection and pulmonary embolism and foot deep vein thrombosis, and these complications can be reasons for mortality in patients 3. Stroke is along with weakness, paralysis, numbness, and loss of sensation in the hands and feet at a side of the body and inability in cognitive and speech and visual and balance 4. Patients with moderate to severe stroke are usually hospitalized and the possibility of again stroke at the patient is low but the possibility of dying in the first month after stroke is % 50 5.
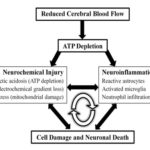
Ischemia influences limit and specific part of the brain, for example, internal capsule, caudate nucleus or cortex by middle cerebral artery occlusion. Also, this event can occur temporarily or permanently. The main Characterize of ischemic is inevitable death during the first minutes after the occurrence in regions that reduced blood flow and consequently ATP level. Then around this area, where there is a small amount of blood flow, occur necrosis 6 as well as neurochemical and neuro-inflammation damages 7 Fig. 1.
FIG. 1: DETRIMENTAL ACUTE EFFECTS OF ISCHEMIC STROKE CAN BE CONCEPTUALIZED INTO TWO SEPARATE BUT HIGHLY INTER-RELATED PHYSIO-LOGICAL ENTITIES, NEUROCHEMICAL AND NEURO-INFLAMMATION INJURY, THAT ULTIMATELY LEAD TO CELLULAR DAMAGE AND DEATH
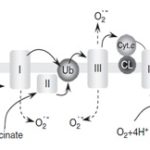
Transient cerebral ischemia is characterized by hypoxia in a short period that then produces large amounts of free radicals during long period of reperfusion. This event leads to the destruction of macromolecules such as proteins, nucleic acids as well as membranes. The result of pathophysiologic is variables and depend on the amount affected intracellular organelles and macromolecules 8. During ischemia, increasing of calcium concentration leads to activation of nitric oxide synthase depended on calmodulin so that non-physiological concentrations of nitric oxide lead to oxidative damage. Also, a combination of superoxide and nitric oxide result in the formation of proxy nitrite and ultimately induction of oxidative damage to macromolecules 9. Another event that occurs during reperfusion is the increase of reactive oxygen species due to reoxygenation so that their accumulations increase the severity of damage 10 Fig. 2.
Nowadays, Studies on the development of neuroprotective agents to treat cerebral ischemia have been focused on antioxidants. Antioxidants have been investigated in many experiments under in-vitro and in-vivo conditions and have also been conducted several clinical trials 11. The antioxidant activity of compounds isolated from plants seems very impressive for example flavonoids are known as an important factor to inhibit lipid peroxidation, platelet aggregation, control fragility and permeability of capillaries, cyclooxygenase and lipoxygenase activities.
FIG. 2: FORMATION OF REACTIVE OXYGEN SPECIES BY THE MITOCHONDRIAL RESPIRATORY CHAIN. CL, CARDIOLIPIN; CYT. C, CYTOCHROME C; UB, UBIQUINONE
These actions are due to their antioxidant effects and their ability to scavenge free radicals 12-14. It has been suggested that antioxidant compounds may prevent cerebral brain damage particularly cerebral damage caused by ischemia/reperfusion. Therefore, it would be interesting argue, studying of effects of antioxidants and free radicals radical scavenger, to obtain protective agents of the brain against cerebral ischemia 15. Here, we reviewed the potential role of compounds derived from plants in the reduction of cerebral ischemia and its complications.
Review Method: In this study, we reviewed papers related to the role of compounds isolated to herb to treat cerebral ischemia. For this purpose, we searched keywords such as plants and cerebral ischemia, natural compounds and cerebral ischemia in databases include a web of science, PubMed and Scopus since from 2000 to 2017.
Natural Compounds and Cerebral Ischemia: Our research group treated rats with transient global cerebral ischemia to metformin as an AMPK activator and determined vascular responses, hyperemia, blood-brain barrier disruption, and electrophysiological activity. The results showed that oral administration of metformin leads to a reduction of blood-brain barrier disruption and reactive hyperemia as well as the increase of spike rates related to electrophysiological records. Our study revealed a regulatory role for AMPK in vascular and electrophysiological responses. Also, metformin can be a useful compound to treat cerebral ischemia 16. In another study, we investigated the effect of metformin in the regulation of inflammatory and antioxidant pathways in rats with global cerebral ischemia. Our findings showed that pretreatment with metformin leads to a reduction of cellular levels of nuclear factor-κB, Tumor Necrosis Factor-alpha, and cyclooxygenase-2; thus it had a potential anti-inflammatory effect. Also, we found that metformin increases levels of Nrf2 and heme oxygenase-1 in the hippocampus. Metformin also increased the level of glutathione and activity of catalase that indicated its anti-oxidant effect 17.
Our other study about the role of metformin to reduce damages of cerebral ischemia on rats with transient forebrain ischemia confirmed that enhancement of sensory-motor signs; anxiolytic behavior and locomotion result from administration of metformin.
Moreover, levels of autophagy factors (light chain 3B, Atg7, Atg5-12, and beclin-1) increased followed by treatment with metformin 18. A research group was shown that metformin pretreatment improved cerebral ischemia induced by 4-vessels occlusion in rats through a reduction of apoptosis and promotion of mitochondrial biogenesis proteins 19. Study on rats with permanent middle cerebral artery occlusion was confirmed that metformin leads to obvious activation of AMPK and induction of autophagy. Also, metformin treatment dramatically reduced infarct volume, neurological deficits and apoptosis.
This study revealed that metformin has an anti-ischemic effect by activation of AMPK in brain 20. Given that, oxidative stress has a pivotal role in inducing damage during the pathogenesis of ischemic; therefore, its abrogation can be a logical idea to treat ischemia. Metformin is one of the compounds to solve this problem because its oral administration to rats with global cerebral ischemia and ischemia/reperfusion improved injuries related to ischemia-reperfusion through the increase of activation of glutathione peroxidase, superoxide dismutase and catalase and reduction of malondialdehyde 21.
In a study, the effect mechanism of gallic acid on cerebral ischemia/reperfusion injury was evaluated, and results showed that gallic acid has a protective effect in rats with cerebral ischemia/reperfusion injury. Also, in-vitro study about the effect of gallic acid on hypoxia / reoxygenation-induced mitochondrial dysfunctions was confirmed that it reduces mitochondrial dysfunction through normalization of mitochondrial membrane potential, mitochondrial permeability transition pore, and ATP level as well as reduction of cell death and ROS level 22. According to our study on the role of gallic acid against cerebral ischemia subsequently, induction of transient global ischemia/reperfusion in rats was revealed that oral administration of gallic acid improves gait performance, sensorimotor disorders, hypoalgesia, and passive avoidance memory. Our study showed that gallic acid had potential Cerebro-protective property 23.
Our study on the effect of ellagic acid against global cerebral ischemia showed that ellagic acid could be a potential compound for management and control cerebral ischemia due to the enhancement of electrocardiogram waves and blood pressure and reduction of MDA level in rats with global cerebral ischemia induced by bilateral vertebral and common carotid arteries occlusion 24. Also, in another study, it has been reported that ellagic acid leads to improvement of neurological deficit and brain weight to body weight ratio. Ellagic acid also normalized lactate dehydrogenase activity and malondialdehyde level in serum while reduced superoxide dismutase activity in rats with focal cerebral ischemia 25. A research group was induced by transient focal cerebral ischemia in rats by middle cerebral artery occlusion, and then animals were treated by crosin.
The results showed that this compound leads to the reduction of infarct volume and brain edema. Also, it had an antioxidant effect so that normalized activity of superoxide dismutase and glutathione peroxidase and reduced malondialdehyde level 26. It has also been reported that oral administration of crosin results increase of activity of superoxide dismutase and glutathione peroxidase and reduction of nitric oxide and malondialdehyde levels and nitric oxide synthase activity in rats with transient focal cerebral ischemia. In addition, crosin abrogated serous edema, vacuolation, membrane damage and mitochondrial damages in cortical microvascular endothelial cells. Evaluation in molecular level revealed that crosin leads to improvement of phosphorylation of extracellular signal-regulated kinase ½ (ERK1/2) and reduction of expression of matrix metalloproteinase-9, oxidizing reactions, and inhibition of GRK2 translocation from the cytosol to the membrane 27.
Study on safranal as an herb active compound was confirmed its anti-ischemic effect against cerebral ischemia-reperfusion-induced by four-vessel occlusion method rats. Indeed, safranal administration leads to increase of total SH contents and antioxidant capacity as well as reduction of TBARS and MDA levels in hippocampus so that these events had a prominent effect of reducing oxidative damage in brain 28. Given that quercetin significantly reduced up-regulation of matrix metalloproteinase-9, blood-brain barrier permeability, and brain edema in rats with focal ischemia induced by photo thrombosis; therefore it is a useful compound for the treatment of cerebral ischemia 29.
Also, it has been reported that quercetin reduces cerebral ischemia neuronal damage in rats with transient focal cerebral ischemia through reduction of infarct size, TBARS level, neuronal loss, and p53 expression, inhibition of the activity of poly (ADP-ribose) polymerase (PARP) and caspase-3 as well as improvement of behaviors deficits 30. Treatment of rats with cerebral ischemic induced by middle cerebral artery occlusion with quercetin leads to the promotion of neurological function and reduction of infarct volume and cell apoptosis. These effects caused by reduction of the number of TdT mediated dUTP nick end labeling positive cells and cleaved caspase-3 protein as well as the increase of expression of BDNF, TrkB and p-Akt 31. Moreover, oral administration of quercetin to rats with chronic cerebral ischemia by bilateral occlusion of the carotid arteries results in promotion of learning and memory performance as well as normalization of long-term potentiation and amplitude of voltage-dependent sodium currents 32.
In a study, the effect of curcumin against cerebral ischemia caused by middle cerebral artery occlusion in rats was evaluated, and results revealed the anti-ischemic effect of curcumin due to the reduction of stress oxidative. Administration of curcumin led to reduction of lipid peroxidation and reduced peroxynitrite formation as well as the increase of activity of superoxide dismutase and glutathione peroxidase in the ipsilateral and contralateral hemisphere. Also, reductions in infarct volume and brain edema were observed 33.
Also, the anti-ischemic effect of curcumin can be related to its antiapoptotic effect because the administration of curcumin to rats with focal cerebral ischemia-reperfusion results in a reduction of cytochrome c releasing and cleaved caspase 3 expression and increase of mitochondrial Bcl-2 expression as well as reduction of malondialdehyde level in the brain. These events had a potential effect of reducing infarct volume and neurological damage 34. In another study, about the role of curcumin in abrogation of damages caused by focal cerebral ischemia in rats was confirmed that curcumin administration leads to up-regulation of Nrf2 and HO-1 as well as reduction of infarct volume, brain water content and behavioral deficits. It seems that to target Nrf2 and HO-1 can be a promising idea to treat cerebral ischemia 35.
Moreover, it has been reported that curcumin protects blood-brain barrier integrity and reduces infarct volume, mortality, water content and extravasation of Evans blue dye in the ipsilateral hemisphere as well as improves in rat’s brain with focal cerebral ischemia/reperfusion.
Also, the study on cultured astrocytes was confirmed inhibition of inducible nitric oxide synthase expression and nitrites/nitrates contents after their increase by lipopolysaccharide/tumor necrosis factor α induction. Another effect of curcumin was an abrogation of ONOO− donor SIN-1-induced cerebral capillaries endothelial cells damage 36. A research group was induced focal cerebral ischemia-reperfusion damage by middle cerebral artery occlusion in rats and then evaluated the effect of curcumin administration. The results showed that curcumin reduces apoptotic by abrogation of expression of caspase-3 protein and followed by TUNEL-positive cells 37. It has been reported that the reason for curcumin anti-ischemic property is its agonist effect on PPARγ.
This property of curcumin leads to the reduction of infarct volume and neuronal damage, suppression of neuroinflammatory response by reduction of IL-1β, TNF-α, PGE2, NO, COX-2, and iNOS in rats with middle cerebral artery occlusion model. Given that, curcumin is a potent PPARγ agonist and subsequently reduced inflammatory response related to cerebral ischemia, therefore, it could be considered as a therapeutic strategy for the treatment of cerebral ischemia damages 38. Experiment on Mongolian gerbils with global cerebral ischemia caused by transient occlusion of the common carotid arteries was showed that curcumin administration reduced neuronal death, glial activation, lipid peroxidation, mitochondrial dysfunction, apoptosis induction and locomotor disability 39.
CONCLUSION: During ischemia, lack of oxygen creates a situation in which bloodstream back leads to the induction of inflammation and oxidative damage rather than normalization of tissue function. Increase of oxygen after the reestablishment of cerebral blood flow has a pivotal role in the formation of free radicals and ultimately deleterious of cell function by cell necrosis and apoptosis. Basic and clinical studies have been indicated that the production of free radicals is one of the most important factors, which leads to cerebral damage, so that oxidative and inflammatory factors significantly increase after cerebral ischemia. Plants are an important source of antioxidants, and natural antioxidants increase plasma antioxidant potency and improvement of diseases such as cancer, heart disease, and stroke. Due to their toxicity and the aberrant effects of synthesized antioxidants, it can be a dire need to reliable sources of antioxidant such herbs because they have properties such as less toxic and more effective.
In conclusion, it can be stated that plant compounds protect the brain against ischemia potential antioxidant activity. Their antioxidant and anti-apoptotic properties may be involved in the protection of neuron during injury induced by cerebral ischemic. Therefore, plants can be ideal candidates to treat cerebral ischemia whether single or co-administration intervention. However, there are still many questions in this area so that their revealing depended on future studies.
ACKNOWLEDGEMENT: Us acknowledgment and gratefulness at the beginning and at last is to God who gave us the gift of the mind. The authors thank Young Researchers and Elite Club, Yasooj Branch, Islamic Azad University due to cooperation in this study.
CONFLICT OF INTEREST: The authors declare that there is no conflict of interest regarding this study.
FINANCIAL SUPPORT AND SPONSORSHIP: This study was supported by the authors named in this article.
ETHICAL APPROVAL: This research did not contain any studies with human participants or animals and was performed by the authors alone.
REFERENCES:
- Thorvaldsen P, Asplund K, Kuulasmaa K, Rajakangas AM and Schroll M: Stroke incidence, case fatality, and mortality in the WHO Monica project. Stroke 1995; 26(3): 361-67.
- Toole JF, Murros K and Veltkamp R: Cerebrovascular disorders. Lippincott Williams & Wilkins, Fifth Edition 1999.
- Ghandehari K: Relation of weakness region and cerebral infarct topography. Daneshvar Medicine 2002; 10(41): 33-36.
- Ghandehari K: Relationship of aphasia and topography of cerebrovascular territories. Scientific Journal of Hamadan University of Medical Sciences 2004; 11(3): 12-15.
- Mohr J, Grotta JC, Wolf PA, Moskowitz MA, Mayberg MR and Von Kummer R: Stroke: Pathophysiology, diagnosis, and management. Saunders, Fifth Edition 2011.
- Astrup J, Siesjö BK and Symon L: Thresholds in the cerebral ischemia-the ischemic penumbra. Stroke 1981; 12(6): 723-25.
- Cai PY, Bodhit A, Derequito R, Ansari S, Abukhalil F and Thenkabail S: Vagus nerve stimulation in ischemic stroke: old wine in a new bottle. Frontiers in Neurology 2014; 5(107): 1-8. DOI: 3389/fneur.2014. 00107
- Beckman JS, Beckman TW, Chen J, Marshall PA and Freeman BA: Apparent hydroxyl radical production by peroxynitrite: Implications for endothelial injury from nitric oxide and superoxide. Proceedings of the National Academy of Sciences of the United States of America 1990; 87(4): 1620-24.
- Dawson VL, Dawson TM, London ED, Bredt DS and Snyder SH: Nitric oxide mediates glutamate neurotoxicity in primary cortical cultures. Proceedings of the National Academy of Sciences of the United States of America 1991; 88(14): 6368-71.
- Orrenius S: Reactive oxygen species in mitochondria-mediated cell death. Drug Metabolism Reviews 2007; 39(2-3): 443-55.
- Margaill I, Plotkine M and Lerouet D: Antioxidant strategies in the treatment of stroke. Free Radical Biology & Medicine 2005; 39(4): 429-43.
- Rafieian-Kopaei M, Baradaran A and Rafieian M: Plant’s antioxidants: From laboratory to clinic. Journal of Nephropathology 2013; 2(2): 152-53.
- Middleton E, Kandaswami C and Theoharides TC: The effects of plant flavonoids on mammalian cells: implications for inflammation, heart disease, and cancer. Pharmacological Reviews 2000; 52(4): 673-51.
- Rafieian-Kopaei M, Baradaran A and Rafieian M: Oxidative stress and the paradoxical effects of antioxidants. Journal of Research in Medical Sciences 2013; 18(7): 629.
- Baradaran A, Rabiei Z, Rafieian M and Shirzad H: A review study on medicinal plants affecting amnesia through the cholinergic system. Journal of Herb Med Pharmacology 2012; 1(1): 3-9.
- Farbood Y, Sarkaki A, Khalaj L, Khodagholi F, Badavi M and Ashabi G: Targeting adenosine monophosphate-activated protein kinase by metformin adjusts post-ischemic hyperemia and extracellular neuronal discharge in transient global cerebral ischemia. Microcirculation 2015; 22(7): 534-41.
- Ashabi G, Khalaj L, Khodagholi F, Goudarzvand M and Sarkaki A: Pre-treatment with metformin activates Nrf2 antioxidant pathways and inhibits inflammatory responses through induction of AMPK after transient global cerebral ischemia. Metabolic Brain Disease 2015; 30(3): 747-54.
- Sarkaki A, Farbood Y, Badavi M, Khalaj L, Khodagholi F and Ashabi G: Metformin improves anxiety-like behaviors through AMPK - dependent regulation of autophagy following transient forebrain ischemia. Metabolic Brain Disease 2015; 30(5): 1139-50.
- Ashabi G, Khodagholi F, Khalaj L, Goudarzvand M and Nasiri M: Activation of AMP-activated protein kinase by metformin protects against global cerebral ischemia in male rats: Interference of AMPK/PGC-1α pathway. Metabolic Brain Disease 2014; 29(1): 47-58.
- Jiang T, Yu JT, Zhu XC, Wang HF, Tan MS and Cao L: Acute metformin preconditioning confers neuroprotection against focal cerebral ischemia by pre-activation of AMPK-dependent autophagy. British Journal of Pharmacology 2014; 171(13): 3146-57.
- Abd-Elsameea AA, Moustaf AA and Mohamed AM: Modulation of the oxidative stress by metformin in the cerebrum of rats exposed to global cerebral ischemia and ischemia/reperfusion. European Review for Medical and Pharmacological Sciences 2014; 18(16): 2387-92.
- Sun J, Ren DD, Wan JY, Chen C, Chen D and Yang H: Desensitizing mitochondrial permeability transition by erk-cyclophilin D axis contributes to the neuroprotective effect of gallic acid against cerebral ischemia/reperfusion injury. Frontiers in Pharmacology 2017; 8: 184.
- Farbood Y, Sarkaki A, Hashemi S, Mansouri MT and Dianat M: The effects of gallic acid on pain and memory following transient global ischemia/reperfusion in Wistar rats. Avicenna Journal of Phytomedicine 2013; 3(4): 329-40.
- Hoseinynejad K, Dianat M, Sarkaki A, Gharibnaseri MK, Badavi M and Farbood Y: Ellagic acid improves electrocardiogram waves and blood pressure against global cerebral ischemia rat experimental models. Electronic Physician 2015; 7(4): 1153-62.
- Kannan MM and Quine SD: Ellagic acid ameliorates isoproterenol induced oxidative stress: Evidence from electrocardiological, biochemical and histological study. European Journal of Pharmacology 2011; 659(1): 45-52.
- Shanbhag NC, Henning RH and Schilling L: Long-term survival in permanent middle cerebral artery occlusion: a model of malignant stroke in rats. Scientific Reports 2016; 6: 28401.
- Kumar V, Bhat ZA, Kumar D, Khan NA, Chashoo IA and Shah MY: Pharmacological profile of Crocus sativus - a comprehensive review. Pharmacol online 2011; 3: 799-11.
- Samarghandian S, Azimi-Nezhad M and Samini F: Preventive effect of safranal against oxidative damage in aged male rat brain. Experimental Animals 2015; 64(1): 65-71.
- Lee JK, Kwak HJ, Piao MS, Jang JW, Kim SH and Kim HS: Quercetin reduces the elevated matrix metalloproteinases-9 level and improves functional outcome after cerebral focal ischemia in rats. Acta Neurochirurgica 2011; 153(6): 1321-29.
- Ahmad A, Khan MM, Hoda MN, Raza SS, Khan MB and Javed H: Quercetin protects against oxidative stress associated damages in a rat model of transient focal cerebral ischemia and reperfusion. Neurochemical Research 2011; 36(8): 1360-71.
- Yao RQ, Qi DS, Yu HL, Liu J, Yang LH and Wu XX: Quercetin attenuates cell apoptosis in focal cerebral ischemia rat brain via activation of BDNF-TrkB-PI3K/Akt signaling pathway. Neurochemical Research 2012; 37(12): 2777-86.
- Sarkaki A, Fathimoghaddam H, Mansouri SM, Korrani MS, Saki G and Farbood Y: Gallic acid improves cognitive, hippocampal long-term potentiation deficits and brain damage induced by chronic cerebral hypoperfusion in rats. Pakistan Journal of Biological Sciences 2014; 17(8): 978-90.
- Altinay S, Cabalar M, Isler C, Yildirim F, Celik DS and Zengi O: Is chronic curcumin supplementation neuroprotective against ischemia for antioxidant activity, neurological deficit, or neuronal apoptosis in an experimental stroke model? Turkish Neurosurgery 2017; 27(4): 537-45.
- Dohare P, Garg P, Sharma U, Jagannathan NR and Ray M: Neuroprotective efficacy and therapeutic window of curcuma oil: in rat embolic stroke model. BMC Complementary and Alternative Medicine 2008; 8: 55.
- Liu Y, Chen L, Shen Y, Tan T, Xie N, Luo M: Curcumin ameliorates ischemia-induced limb injury through immunomodulation. Medical Science Monitor 2016; 22: 2035-42.
- Kannappan R, Gupta SC, Kim JH, Reuter S and Aggarwal BB: Neuroprotection by spice-derived nutraceuticals: you are what you eat!. Molecular Neurobiology 2011; 44(2): 142-59.
- Li W, Suwanwela NC and Patumraj S: Curcumin prevents reperfusion injury following ischemic stroke in rats via inhibition of NF‑κB, ICAM-1, MMP-9 and caspase-3 expression. Molecular Medicine Reports 2017; 16(4): 4710-20.
- Cheng CY and Lee YC: Anti-Inflammatory Effects of Traditional Chinese Medicines against Ischemic Injury in in-vivo Models of Cerebral Ischemia. Evidence-based Complementary and Alternative Medicine 2016. doi: 10.1155/2016/5739434
- Lee SH, Ko IG, Kim SE, Hwang L, Jin JJ, Choi HH: Aqueous extract of Cordyceps alleviates cerebral ischemia-induced short-term memory impairment in gerbils. Journal of Exercise Rehabilitation 2016; 12(2): 69-78.
How to cite this article:
Hassanpour SH and Karami SZ: The role of herbal compounds in the treatment of cerebral ischemia. Int J Pharmacognosy 2018; 5(3): 117-22. doi link: http://dx.doi.org/10.13040/IJPSR.0975-8232.IJP.5(3).117-22.
This Journal licensed under a Creative Commons Attribution-Non-commercial-Share Alike 3.0 Unported License.
Article Information
1
117-122
595
1439
English
IJP
S. H. Hassanpour * and S. Z. Karami
Young Researchers and Elite Club, Yasooj Branch, Islamic Azad University, Yasooj, Iran.
Dr.hossein1366@yahoo.com
10 October 2017
12 November 2017
18 November 2017
10.13040/IJPSR.0975-8232.IJP.5(3).117-22
01 March 2018