COMPARISON, FORMULATION DEVELOPMENT AND BASIC EVALUATION OF IN-VITRO ANTI-UROLITHIATIC POTENTIAL OF OCIMUM TENUIFLORUM AND MENTHA PIPERITA MEDICINAL PLANT SPECIES
HTML Full TextCOMPARISON, FORMULATION DEVELOPMENT AND BASIC EVALUATION OF IN-VITRO ANTI-UROLITHIATIC POTENTIAL OF OCIMUM TENUIFLORUM AND MENTHA PIPERITA MEDICINAL PLANT SPECIES
Jasmeen Syan * and Chandra Shekhar Tailor
School of Pharmaceutical Sciences, Shri Guru Ram Rai University, Patel Nagar, Dehradun, Uttarakhand, India.
ABSTRACT: Urolithiasis or kidney stones is defined as a urinary stone originating anywhere in the urinary tract. Urolithiasis plays a significant economic burden in the healthcare system, especially in developing countries, owing to changes in food habits and lifestyle due to a significant increase in the disease over the last few decades. Medicinal plants are established as renewable sources with antiurolithiatic activity. There are many Marketed formulations with Antiurolithiatic activity as well as many traditional medicinal plants primarily used to dissolve urinary stones in the kidney or urinary bladder. The comparative study of Ocimum and Mentha plant species is carried out for studying In-vitro ant-urolithiatic activity. Further, the extract showing the most prominent activity is taken, and formulation syrup is prepared. This study is based on studying the in-vitro Anti urolithiatic potential of Ocimum tenuiflorum Linn. and Mentha piperita Linn. belonging to the family Lamiaceae.
Keywords: Kidney stones, Urolithiasis, Syrup, Extraction, Medicinal plants
INTRODUCTION: To treat infectious and non-infectious, the modern healthcare system offers a wide range of possibilities. However, due to cost and accessibility concerns, some of these medications have their drawbacks and are not available to most of the world’s population. As a result, more than 75% of people, particularly in lower-income nations, still rely on herbal treatments to address their basic medical needs 1. Medicinal plants play a significant role in the health care of ancient and modern cultures.
Ayurveda, the Indian system of medicine, mainly uses plant-based formulations to treat various human diseases because they contain the components of therapeutic potential. Plant-based drugs are an important source of therapeutic agents because of their abundant availability, relatively cheaper cost, and non-toxic nature when compared to modern medicine 2.
It is important to consider traditional remedies for non-life-threatening conditions, including haemorrhoids and urinary stones. Urolithiasis is a disorder in which a stone forms or occurs anywhere in the urinary tract. Urinary stones (calculi) are solid crystalline masses that can form anywhere in the renal tract 3. Stone formation is a painful urologic disease that occurs in around 12% of the global population, and its occurrence rate in males is 70-81% and 47-60% in females. It is assessed that at least 10% of the population in industrialized parts suffer from urinary stone formation. The occurrence of renal calculi is less in the southern part when compared with other parts.
Stone formation usually occurs due to insufficient urinary discharge, microbial infection in the urinary tract, diet with excess oxalates and calcium, vitamin abnormalities like vitamin A deficiencies, excess vitamin D, and metabolic diseases like hyperthyroidism, cystinuria, gout, intestinal dysfunction etc. Kidney stone formation or urolithiasis is a complex procedure due to an imbalance between promoters and inhibitors in the kidneys 4.
The use of plant products with claimed uses in the traditional systems of medicine assumes importance. In the Ayurvedic system of medicine in India, plants belonging to ‘Pashanabheda’ group are claimed to be useful in treating urinary stones. ‘Pashanabheda’ is the Sanskrit term used for a group of plants with diuretic and antiurolithiatic activities 5.
Stone formation is a complex process resulting from several physicochemical properties, including supersaturation, crystal nucleation, precipitation, crystal growth, crystal aggregation, and urinary stone constituents' retention within tubular cells. There are various kidney stones, including cystine, calcium oxalate, calcium phosphate, struvite, and uric acid stones. However, crystal retention, cell apoptosis, renal cell injury, and associated stone promoters or inhibitors play important roles in kidney stone formation 6.
Types of Kidney Stones 7, 8, 9:
Calcareous Stones (Calcium Containing Stones):
Calcium Oxalate Stones: The most common type of kidney stone which is created when calcium combines with oxalate in the urine. Inadequate calcium and fluid intake and other conditions may contribute to their formulations. Calcium oxalate stones occur as a result of.
- Hypercalciuria: This is idiopathic or results from any disorder that induces even mild hypercalcemia.
- Hypocitraturia: Citrate is an inhibitor of calcium salt formation by forming a soluble complex with calcium. It results from causes of intracellular acidosis such as renal failure, potassium deficiency, distal renal tubular acidosis, chronic diarrhoeal state, and drugs such as acetazolamide.
- Hyperuricosuria: It occurs at high purine intake or chronic diarrhoeal disease.
- Hyperoxaluria: Oxalate forms an insoluble complex with calcium, resulting in crystal formation.
Calcium Phosphate Stones: It occurs when the kidney loses its ability to lower urinary pH, causing calcium phosphate supersaturation.
Non-Calcareous Stones:
Uric Acid Stones: This is another common type of kidney stone. High purine intake leads to a higher production of monosodium urate may form kidney stones. Uric acid composition seems to be the second most common stone. Urinary uric acid is insoluble at pH ˂ 5.05 and forms crystals.
Struvite Stones: Struvite is a crystalline substance composed of magnesium ammonium phosphate. These stones are less common and are caused by infections in the upper urinary tract.
Cystine Stones: When the kidney does not reabsorb the cystine properly leads to kidney stones. The stones are greenish-yellow, flecked with shiny crystallites, and moderately opaque with a rounded appearance.
MATERIAL AND METHODS:
Collection and Authentification of Ocimum tenuiflorum Linn. and Mentha piperita Linn. Medicinal plant Species: Fresh leaves of both plant species were collected from Dehradun region and authenticated from the Botanical Survey of India (BSI) Dehradun, Uttarakhand, under Accession numbers: 1335 & 1336. The leaves were washed to remove any kind of dirt.
Preparation of Various Extracts using both Plant species Ocimum tenuiflorum Linn. and Mentha piperita Linn: Fresh leaves were used for the extraction. The leaves were collected and washed. To obtain a constant weight the leaves were crushed properly. Extraction from Ocimum tenuiflorum and Mentha piperita was done using 25gm with 250 ml of water for aqueous extract by Maceration method and Chloroform and ethanol by Soxhlet method. The extracts were concentrated in a water bath until it was completely dried. The dry extract was kept in a sealed beaker 10.
Preliminary Phytochemical Screening of both Plant Species: General tests for the Presence of Alkaloids, Glycosides, Tannins, Saponins and Phenolic compounds were conducted.
Test for Alkaloids:
Drangendroff’s test: To 2-3ml extract, a few drops of Drangendroff’s reagent was added, giving Orange brown ppt.
Mayer’s test: To 2-3ml extract, few drops of Mayer’s reagent were added, giving White ppt.
Wagner’s test: To 2-3ml extract, a few drops of Wagner’s reagent are added, giving Reddish brown ppt.
Hager’s test: To 2-3 ml extract, a few drops of Hager’s reagent added, giving yellow ppt.
Test for Flavonoids:
Sulphuric Acid test: On addition of sulphuric acid, flavonoids dissolve and give deep yellow solution.
Lead Acetate test: To the residue, lead acetate solution was added. Yellow coloured precipitate formed.
Zinc HCl test: Test solution was heated with Zinc and HCl. Pink to red colour appeared.
Shinoda test: Test solution was treated with few fragments of magnesium ribbon and conc. HCl showed pink to magenta red colour.
Test for Glycosides:
Killer-Killani test: To the extract, Glacial acetic acid, 1 drop 5% FeCl3 & conc. H2SO4 were added. Reddish brown colour appeared at junction of two liquid layers & upper layer appeared bluish green.
Legal’s test: To the extract, 1ml of pyridine and 1 ml of Sodium nitroprusside were added giving Pink to red colour.
Baljet’s test: Sodium picrate was added to the extract, which gives yellow to orange colour.
Bromine Water test: Bromine water was added to the extract, which gives yellow precipitate.
Test for Saponins:
Foam test: Extract was shaken vigorously with water. Foam observed.
Haemolytic test: Extract was added to one drop of blood placed on glass slide. Haemolytic zone appeared.
Test for Phenols & Tannins: To 2-3 ml of extract, few drops of following reagents added:
Lead Acetate Solution: White ppt. observed.
5%FeCl3 Solution: Deep blue-black colour observed.
Acetic Acid Solution: Red colour observed.
Dilute HNO3 test: Reddish to yellow colour observed.
Dilute Iodine test: Transient red colour observed.
In-vitro Comparative Study of the Anti- Urolithiatic Activity of both Ocimum tenuiflorum and Mentha piperita all Extracts:
Preparation of Calcium Oxalate Crystals by Homogenous Precipitation: Equimolar solutions of Calcium chloride dihydrate dissolved in distilled water and Sodium oxalate dissolved in 10 ml of 2N H2SO4 and distilled water were prepared. A sufficient quantity was allowed to react in a beaker with slight aid of heat until more ppt occurred.
The resulting ppt was Calcium oxalate, freed from traces of sulfuric acid by treating with ammonia solution. Finally, it was washed with distilled water and dried at a temperature 60° C for 4 hrs.
Preparation of Semi-Permeable Membrane from Farm Eggs: Shell was removed chemically by placing the eggs in 2M HCl for 24 hrs, which caused complete decalcification.
Further, the contents squeezed out completely from the decalcified egg. It was washed thoroughly with distilled water, and placed in ammonia solution in the moistened condition for a while. Finally, it is stored in Refrigerator at a pH of 7-7.4.
Method: A total of 8 semi-permeable membranes were prepared. Exactly 1 mg of Calcium oxalate and 10 mg of various drug extracts and standard were weighed and packed in semi-permeable membrane separately and carefully sutured. This was allowed to suspend in a conical flask containing 100 ml of 0.1M TRIS buffer. All the conical flasks were maintained at room temperature undisturbed for 7-8 hours. The contents were transferred into a test tube and 2 ml of 1N Sulfuric acid was added and titrated with KMnO4 till a light pink colour was obtained 13, 14.
TABLE 1: DIFFERENT PLANT EXTRACTS GROUPS
| S. no. | Group No. | Treatment Details | |
| 1. | Group 1 | MCE | Mentha Chloroform extract |
| 2. | Group 2 | MEE | Mentha Ethanolic extract |
| 3. | Group 3 | MAE | Mentha Aqueous extract |
| 4. | Group 4 | OCE | Ocimum Chloroform extract |
| 5. | Group 5 | OEE | Ocimum Ethanolic extract |
| 6. | Group 6 | OAE | Ocimum Aqueous extract |
| 7. | Group 7 | STD | Neeri Syrup |
| 8. | Group 8 | Control | ---------- |
FIG. 1: CONICAL FLASKS CONTAINING TRIS BUFFERS ALONG WITH EGG MEMBRANES
FIG. 2: BEAKERS CONTAINING FARM EGGS FOR DECALCIFICATION
Formulation using Chloroform extract of Ocimum and Mentha: The ingredient mentioned in Table 2 were taken in a beaker and heated until a thick syrup solution was formulated.
TABLE 2: INGREDIENTS USED IN SYRUP FORMULATION FOR ANTI-UROLITHIATIC POTENTIAL
| S. no. | Name of the Ingredient | Amount used |
| 1. | Ocimum Chloform extract | 2ml |
| 2. | Mentha Chloroform extract | 2ml |
| 3. | Sucrose | 66.66gm |
| 4. | Methyl Parabeen | 2gm |
| 5. | Sodium benzoate | 2gm |
| 6. | Sodium chloride | 2gm |
| 7. | Sweet Orange flavor | 3-4 drops |
| 8. | Distilled water | q.s |
Evaluation Parameters of Syrup Formulation:
Colour: The syrup was taken and placed against a white background in white tube light and observed through naked eye.
Odour: Observed by Sense of smell.
Taste: It was determined by the tongue.
Determination of pH: The pH was determined using pH meter.
Determination of viscosity- Viscometer was used to determine the viscosity of syrup 15, 16.
In-vitro Assessment of Anti Urolithiatic Activity of Prepared Syrup Formulation using:
Chloroform Extracts of Mentha and Ocimum Plant species: The activity was observed by titration as mentioned earlier and compared with Standard formulation.
RESULTS AND DISCUSSION:
Preliminary Phytochemical screening of Ocimum tenuiflorum L. and Mentha piperita L.
TABLE 3: PHYTOCHEMICAL SCREENING OF OCIMUM TENUIFLORUM LINN
| S. no. | Contents | Aqueous Extract | Chloroform Extract | Alcoholic Extract |
| 1. | Alkaloids | + | + | + |
| 2. | Tannins | + | + | + |
| 3. | Saponin | + | + | + |
| 4. | Flavonoids | + | + | + |
| 5. | Glycosides | - | _ | _ |
| 6. | Proteins | + | + | + |
(+) Present (-) Absent.
TABLE 4: PRELIMINARY PHYTOCHEMICAL SCREENING OF MENTHA PIPERITA LINN.
| S. no. | Contents | Aqueous Extract | Chloroform Extract | Alcoholic Extract |
| 1. | Alkaloids | + | + | + |
| 2. | Tannins | + | + | + |
| 3. | Flavonoids | + | + | + |
| 4. | Saponin | + | + | + |
| 5. | Proteins | - | _ | _ |
| 6. | Glycosides | + | + | + |
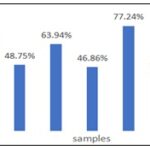
In-vitro Comparative Study of Anti- Urolithiatic Potential of both Ocimum tenuiflorum and Mentha piperita Extracts: The Chloroform extract of the Ocimum and Mentha was found to be the most significant to possess anti-urolithiatic potential which dissolved Calcium oxalate crystals significantly when compared to other extracts. The result of the extracts is depicted in Table 4.
TABLE 5: AMOUNT OF % CALCIUM OXALATE DISSOLVED BY EXTRACTS
| S. no. | Extracts | Amount of Calcium Oxalate Dissolved |
| 1. | MCE | 60.14% |
| 2. | MAE | 43.56% |
| 3. | MEE | 48.75% |
| 4. | OCE | 63.94% |
| 5. | OAE | 58.24% |
| 6. | OEE | 46.86% |
| 7. | STD | 77.24% |
| 8. | Control | ------ |
As the Chloroform extracts have the most potential activity it depicts that the ability to dissolve calcium stone of the Chloroform extracts are the most. The increasing order of Anti urolithiatic activity with various extracts tested was STD> OCE> MCE>OAE>MEE>OEE>MAE.
FIG. 3: GRAPH REPRESENTING ANTI-UROLITHIATIC ACTIVITY AS % OF CALCIUM OXALATE DISSOLVED BY VARIOUS EXTRACTS
Evaluation Parameters of Syrup Formulation:
Colour: Green
Odour: Characteristic
Taste: Sweet
pH: 6.5
Viscosity: 0.09 poise
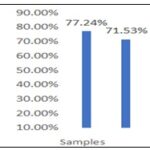
In-vitro Assessment of Anti-urolithiatic Potential of Prepared Syrup formulation using both Ocimum and Mentha Plant species Chloroform Extracts: The Syrup formulation was prepared, and the amount of Calcium oxalate dissolved was found to be 71.53% compared to the standard which was 77.24%.
FIG. 4: GRAPH REPRESENTING ANTI-UROLITHIATIC POTENTIAL AS % OF AMOUNT OF CALCIUM OXALATE DISSOLVED BY SYRUP FORMULATION AND STANDARD MARKETED FORMULATION NEERI SYRUP
CONCLUSION: For optimum patient treatment and Protection, Scientific Research exploring potential benefits of herbal plants is extremely important. The Present article demonstrated the curative potential of Urolithiasis or kidney stones using traditional medicinal plants. This study aims to represent the medicinal plants of Lamiaceae used in anti-urolithiatic activity, followed by a comparative study of extracts of both Plant species. After comparison, the formulation was prepared and evaluated with the standard marketed NEERI Syrup for the Anti-urolithiatic activity. More research is needed to carry out this research on animal models and to develop more new plant-derived products to treat the formation of kidney stones.
ACKNOWLEDGEMENT: The Authors are thankful to SGRR Education mission and Chairman of Mission, Shri Mahant Devendra Dass Ji Maharaj, along with the Vice-Chancellor and Dean of School of Pharmaceutical Sciences for their kind support and motivation to carry out this research work in the department.
CONFLICTS OF INTEREST: We also declare that all ethical guidelines have been followed during this work, and there is no conflict of interest among authors.
REFERENCES:
- Nimavat A, Trivedi A, Yadav A and Patel P: a review on kidney stone and its herbal treatment. Journal of Pharmacy and Pharmacology 2022; 10: 195-209.
- Agbor AG and Ngogang YJ: Toxicity of herbal preparations. Cam J Ethnobot 2005; 1: 23-28.
- Pareek SK: “Medicinal Plants in India: Present Status and Future Prospects” In: Prospects of Medicinal Plants 1996; 14.
- Shukla AK, Shukla S, Garg A and Garg S: “A Review on anti-urolithiatic activity of herbal folk plants” Asian Journal of Biomaterial Research 2017; 3(2): 1-1.
- Nagal A and Singla RK: “Herbal resources with antiurolithiatic effects: a Review” Indo Glob J Pharm Sci 2013; 3(1): 6-14.
- Butterweck V and Khan SR: Herbal medicines in the management of urolithiasis: alternative or complementary. Planta Med 2009; 75(10): 1095-1103.
- Fontenelle LF and Sarti TD: Kidney stones: treatment and prevention. American Family Physicia 2019; 99(8): 490-6.
- Frassetto L and Kohlstadt I: Treatment and prevention of kidney stones: an update. American Family Physician 2011; 84(11): 1234-42.
- Knoll T: Epidemiology, Pathogenesis and Pathophysiology of urolithiasis. Europe Urol Supplem 2010; 9(12): 802-06.
- Niharika M, Suchitha N, Akhila S, Himabindhu J and Ramanjaneyulu K: Evaluation of in-vitro antiurolithiatic activity of Gossypium herbaceum. J of Pharmaceutical Sciences and Research 2018; 10(5): 1236-7.
- Niharika M, Harshitha V, Ashwini P, Srivinya B, Himabindhu J and Ramanjaneyulu K: Evaluation of in-vitro antiurolithiatic activity of Chlorisbarbata. International J of Current Pharma Res 2018; 10(3): 65-7.
- Suvarna Y and Rahaman SK: In-vitro and in-vivo evaluation of antiurolithiatic activity of piperine from Piper nigrum. Research Journal of Pharmacy and Technology 2019; 13(1): 63-8.
- Karunasree V, Sushmitha M, Urmila SS and Sravya R: Assessment of Potential Antiurolithiatic Activity of Some Selected Medicinal Plants by in-vitro Techniques”. Acta Sci Pharma Sci 2017; 1: 38-42.
- Radhasinganallur Ramu, Ravi Doraiswamy and Hiran Mai Yadav: Antiurolithiatic activity of aqueous bark extract of Crateva Magna Lour. (DC). International Journal of Research in Ayurveda and Pharmacy 2017; 8: 271-278.
- Suvarna Y and Rahaman SA: Formulation, evaluation, and study of antiurolithiatic activity of piperine syrup. Drug Invent Today 2020; 13(2): 163-7.
- Thangarathinam N, Jayshree N, Metha AV and Ramanathan L: Development, standardization and evaluation of a polyherbal syrup. International Journal of Pharmaceutical Sciences Review and Research 2013; 20(2): 149-54.
How to cite this article:
Syan J and Tailor CS: Comparison, formulation development and basic evaluation of in-vitro anti-urolithiatic potential of Ocimum tenuiflorum and Mentha piperita medicinal plant species. Int J Pharmacognosy 2023; 10(6): 324-29. doi link: http://dx.doi.org/10.13040/IJPSR.0975-8232.IJP.10(6).324-29.
This Journal licensed under a Creative Commons Attribution-Non-commercial-Share Alike 3.0 Unported License.
Article Information
4
324-329
608 KB
805
English
IJP
Jasmeen Syan * and Chandra Shekhar Tailor
School of Pharmaceutical Sciences, Shri Guru Ram Rai University, Patel Nagar, Dehradun, Uttarakhand, India.
jasminsyan1@gmail.com
27 May 2023
18 June 2023
20 June 2023
10.13040/IJPSR.0975-8232.IJP.10(6).324-29
30 June 2023