BIOGLASS AND HERBAL THERAPEUTICS: A REVOLUTIONARY APPROACH TO ENHANCING ORAL HEALTH MANAGEMENT
HTML Full TextBIOGLASS AND HERBAL THERAPEUTICS: A REVOLUTIONARY APPROACH TO ENHANCING ORAL HEALTH MANAGEMENT
Riya Dsilva, Arti Gachake and Vaibhav Shinde *
Department of Pharmacognosy, Poona College of Pharmacy, Erandwane, Pune, Maharashtra, India.
ABSTRACT: In recent decades, oral health management has witnessed a paradigm shift by integrating bioactive materials into dental therapeutics. Among these, bioactive glasses (BGs) that were originally developed by Larry Hench in 1969 have garnered significant attention because of their distinctive capacity to bond with bones and soft tissues of the body, while stimulating biological responses that promote healing and regeneration. Bioglass was the first synthetic material that formed a chemical bond with bone. The principal mechanism underlying the bioactivity of BGs lies in their surface reactions in aqueous environments, where they release therapeutic ions like Ca²⁺, Na⁺, PO₄³⁻, and Si⁴⁺, that lead to the formation of a hydroxycarbonate apatite (HCA) layer that mimics natural bone mineral. Furthermore, functionalization of bioactive glasses (BGs) with therapeutic metal ions like Ag⁺, Zn²⁺, Cu²⁺, Sr²⁺ and herbal bioactives has emerged as a promising strategy to enhance their antimicrobial, osteogenic, angiogenic, and anti-inflammatory properties, thereby broadening their applications in dental and ocular implantology, orthopedics, and wound healing. Despite the widespread recognition of its benefits, the translation of BGs into mainstream clinical practice has been limited by challenges related to mechanical strength, processing focused on the development of mesoporous Bioglasses, nanostructured BGs, and BG-polymer composites, aiming to optimize their handling characteristics, bioactivity, and controlled drug delivery capabilities. This review intends to highlight the in in-depth analysis of Bioglass in the management of oral health, covering its mechanisms of action, therapeutic potential, clinical outcomes, and emerging innovations.
Keywords: Bioglass, Dental caries, Dentin hypersensitivity, Herbs doped Bioglass, Oral health
INTRODUCTION: Oral health is a fundamental component of overall well-being, encompassing the health of teeth, gums, and the entire oral-facial system that enables essential functions such as speaking, smiling, chewing, and expressing emotions1.
According to the World Health Organization (WHO), oral diseases affect approximately 3.5 billion people worldwide, with untreated dental caries (tooth decay) in permanent teeth being the most common issue.
Recognising the significant burden possessed by oral diseases, the WHO has developed a Global Oral Health Action Plan for 2023–2030. This plan outlines strategic objectives and actions aimed at improving oral health on a global scale. It emphasizes integrating oral health into universal health coverage, promoting preventive care, and addressing common risk factors such as tobacco use, unhealthy diets, and harmful alcohol consumption 2. Maintaining optimal oral health is challenging due to various factors. Primarily, the socioeconomic disparities limit their approach to dental care, which disproportionately affect marginalised and low-income groups who are more likely to suffer from periodontal diseases and dental caries 3. Poor oral hygiene, infrequent dental visits, and high sugar intake also contribute to declining oral health. Systemic conditions like diabetes and cardiovascular diseases can worsen oral issues, highlighting the link between oral and general health 4. Mental health disorders like depression, negatively impact personal care and oral hygiene habits 5. Moreover, oral health is impacted not only by systemic health conditions and disorders but also by hormonal fluctuations during pregnancy, which can lead to a deterioration of oral health, including an increased risk of gingivitis and periodontitis 6. To address these issues, a variety of oral care formulations are available to maintain oral hygiene and prevent dental diseases that include toothpastes, mouthwashes, gels, and chewing gums containing active agents such as fluoride, triclosan, cetylpyridinium chloride, and essential oils 7. However, the modern dental science is moving beyond the use of traditional, inert materials towards a new generation of innovative biomaterials. One such bioactive material that has significantly contributed in healing bone defects and restorative oral surgeries is Bioglass 8. It has a unique and potent property of bioactivity that helps to form a rapid and robust bond with bone and soft tissues 9. Bioglass is a pioneering bioactive material that has transformed the landscape of oral health care by offering unique regenerative and antimicrobial properties 10. Originally developed for bone repair, Bioglass has found extensive applications in dentistry because of its capacity to adhere to both soft and hard tissues, promote mineralisation in dental implants, alleviate dentin hypersensitivity, and promote tissue and craniofacial regeneration 11–13. This is very crucial in treating a wide variety of oral and dental issues, unlike the other oral treatment alternatives like fluoride, triclosan, chlorhexidine, etc that usually have adverse effects associated with their therapeutic use.
Brief History and the Bioglass Revolution: The history of Bioglassdates back to the 1960s with the ground breaking work of Professor Larry Hench, who sought to develop a material that could form a living bond with bone 14. At that time, metals were commonly used as implants in orthopaedic surgeries. However, over time, these metals would corrode inside the body, posing health risks and potentially causing toxicity 15. This led to the development of the first-generation Bioglass, known as 45S5, which demonstrated a remarkable ability to stimulate bone growth, representing a major shift from the inert materials previously used. This silica-based material bonds directly to bone and stimulates gene activation for osteogenesis within 48 hours of implantation, promoting rapid bone regeneration. This unique bioactivity redefined implant material goals, emphasizing natural healing processes, making Bioglass a cornerstone in biomaterials science and the field of bioactive ceramics 16. Subsequent advancements over the following decades focused on tailoring Bioglass compositions to control their degradation rates and improve their mechanical properties for specific applications like wound healing, tissue engineering and the multifaceted world of oral health 17. Table 1. Represents the evolution of Bioglass over decades and its significant characteristics.
TABLE 1: EVOLUTION OF BIOGLASS
| Year | Significance | Details |
| 1969 | Discovery of Bioglass | Development of 45S5 Bioglass by Sir Larry Hench that bonded with bone tissue 18 |
| 1970-1980 | Conduction of Clinical trials | Clinical trial study proved success of Bioglass in orthopedic and dental implants also avoids immune rejection 19. |
| 1990s | Commercialization of Bioglass | Products like Perioglass and NovaBone enter the market for use in bone grafts and periodontal repair 20 |
| 2000s | Development of Bioglass ceramics | Bioglass with advanced structural features for load-bearing applications 21 |
| 2010 | Advanced applications | Integration with polymers, 3D printing and use in cancer therapy and tissue engineering 22 |
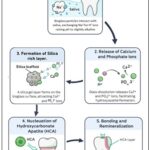
The Fundamental Mechanism of Bioglass Bioactivity: Bioglass is primarily a family of bioactive glasses composed of silicon dioxide, sodium oxide, calcium oxide, and phosphorous pentoxide. These materials exhibit both bioactivity and biodegradability, enabling the controlled release of therapeutic ions that modulate cellular responses. Owing to these properties, they are well-suited for diverse biomedical applications, including bone substitution and replacement, as well as the regeneration of both soft and hard tissues 23. Bioglass can be classified into three primary classes: silicate, borate, and phosphate Bioglass, based on the type of network-forming oxides. They can be synthesized using either the melt quenching method or the sol-gel method 24. Bioglass is typically composed of calcium sodium phosphosilicate, has revolutionized oral care by offering a unique mechanism as described in Fig. 1, that promotes healing and remineralisation of dental tissues. Its bioactivity stems from its ability to interact with bodily fluid like saliva which initiates a cascade of chemical reactions that result in the formation of a mineral layer similar to natural tooth enamel. When Bioglass is introduced into the oral environment, such as through toothpaste or dental treatments, it begins a multi-phase process as represented in Fig. 1.
FIG. 1: MECHANISM OF ACTION OF BIOGLASS ON TOOTH SURFACE
Bioglass and other biomaterials have played a significant role in bone repair for more than 30 years. Their effectiveness is largely attributed to their versatile properties, which can be tailored to enhance specific biological responses in both orthopedic and dental fields. For instance, Bioglass can promote the formation of new bone tissue, facilitate the healing process, and even provide antibacterial effects 25. The formation of Hydroxycarbonate apetite layer (HCA) releases ions like Ca2+, Si4+, Na+, PO43- which directly influence cellular signalling and promote bone regeneration 26.
Moreover, Bioglass can have antimicrobial effects by raising pH and directly inhibiting the progression of caries causing and periodontopathogenic like Streptococcus mutans and Porphyromonas gingivalis 27, 28. Incorporating ions such as lithium, strontium, magnesium, or cerium can further enhance antibacterial and remineralizing properties 29.
Current Treatments for Oral Care: The most commonly used agent in various oral care formulations is Fluoride, which is widely known for its ability to strengthen tooth enamel and prevent dental caries. When used in recommended doses, fluoride is generally considered safe. However, excessive exposure can lead to dental fluorosis, oral irritation, and, in rare cases, systemic toxicity 30, 31.
Another important active ingredient is Triclosan, an antibacterial agent that has shown to improve gingival health and reduce plaque formation when used in dentifrices. However, clinical studies have reported that triclosan-containing oral products can lead to oral mucosal irritation and taste disturbances. Moreover, it is also considered the most common endocrine disruptor 32.
A systematic review highlighted that users of triclosan mouthrinses frequently experienced taste alterations and mucosal irritations, leading to its removal from use in the European Union and the United States 33.
Cetylpyridinium chloride, a quaternary ammonium compound, exhibits antimicrobial properties effective against plaque and gingivitis. While being effective in reducing dental plaque and gingivitis, its prolonged use is associated with several side effects, like tooth and tongue staining and temporary loss or alteration of taste in a few cases 34.
Also, oral burning, taste alterations, ulcers and stomatitis were also reported in some cases 35. Among mouthwashes, chlorhexidine gluconate is considered the gold standard for its broad-spectrum antimicrobial activity and substantivity, making it effective in managing gingivitis and periodontitis. However, its long-term use is associated with side effects such as tooth staining, altered taste sensation, increased calculus formation, and, in rare cases, mucosal irritation 36.
Bioglass is such a bioactive material that significantly surpasses current conventional oral treatment options by actively engaging with biological tissues. It has a distinct ability to release ions like Ca2+, Si4+, and PO43− that directly stimulate cellular regeneration, offer inherent antimicrobial properties by increasing local pH, and can serve as a smart delivery system for therapeutic agents.
This versatile material facilitates true tissue restoration and enhances the stability of dental repairs for a prolonged period of time. It adopts a proactive approach to disease prevention, surpassing the limitations of conventional materials that provide only structural support or temporary relief.
Bioglass in Oral Health: Applications and Latest Advancements: In dentistry, Bioglasshas been explored across multiple disciplines including periodontics, restorative dentistry, endodontics, and implantology 37. Bioactive glasses are beneficial in toothpaste formulation due to their ability to release antibacterial agents, promote remineralization, and reduce hypersensitivity. One such bioactive glass is NovaMin, which serves as an active ingredient in toothpaste to enhance remineralisation and alleviate tooth sensitivity. NovaMin, which is composed of calcium-sodium-phosphate silicate, releases calcium and phosphate ions.
These ions help raise the pH level, facilitating the deposition of calcium phosphate, and its conversion to hydroxyapatite 38. In a study of toothpaste containing fluoride and Bioglass, it was reported that bioactive glass has the potential to prevent mineral loss on bleached enamel 39. In periodontology, BG particles have been successfully used for the regeneration of periodontal tissues, showing comparable or superior results to traditional graft material 40.
In implant dentistry, BG coatings on titanium surfaces promote osseointegration and may prevent peri-implant diseases by modifying the peri-implant microbiome 41. Moreover, its incorporation into dental adhesives and restorative materials offers the potential for enhanced remineralization and antibacterial properties, especially beneficial in managing caries-prone patients 42.
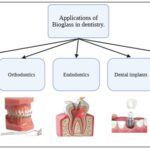
FIG. 2: APPLICATIONS OF BIOGLASS IN DENTISTRY
Dentin Hypersensitivity (DH): Bioglass plays an important role in managing dental hypersensitivity, which is a clinical condition characterised by sharp stabbing pain due to exposed dentin tubules in response to thermal or chemical stimuli 43. There is a perception of pain arising from the stimulation of mechanoreceptors in the dental pulp due to fluid movement within exposed dentinal tubules. Managing DH would require occluding the exposed tubules or modulating the nerve responses 44. The mechanism by which Bioglass alleviates pain associated with dentin hypersensitivity (DH) involves covering exposed dentin tubules. Bioglass has the unique ability to form a hydroxycarbonate apatite (HCA) layer that blocks external stimuli, reducing sensitivity and relieving pain. This biomimetic mineralisation also occludes the tubules and integrates with the natural tooth structure, providing durable relief. Fluoride-containing Bioglass formulations further enhance this effect by forming a fluorapatite layer, which is more resistant to acid attack and offers longer-lasting protection 45.
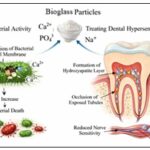
Systemic reviews and in-vitro studies report that when desensitizers like fluoride or gelatin modifications are added to the composition of Bioglass, there is significant reduction in long-term and short-term symptoms of DH 46. The clinical applications of Bioglass in treating dentin hypersensitivity (DH) include its use in toothpastes, desensitizing treatments, and restorative materials. One well-known formulation of Bioglass is NovaMin, which is widely used in dentistry. Studies have shown that NovaMin-containing toothpastes can significantly reduce sensitivity within a few weeks of use, often outperforming traditional agents like potassium nitrate 47. Moreover, Bioglass has shown antimicrobial properties, contributing to improved gingival health and reduced plaque accumulation, which indirectly benefits DH management 48. The Fig. 3, shows the antibacterial effect of Bioglass on remineralisation and treating hypersensitivity 49.
FIG. 3: BIOGLASS IN TREATING DENTIN HYPERSENSITIVITY
In Maxillofacial Surgery and Restorative Dentistry: In the field of maxillofacial surgery, bioactive glass serves as a commonly used bone graft alternative for the restoration of craniofacial defects and the repair of orbital floor injuries 50. Once implanted, it initiates a cascade of surface-level reactions, beginning with the exchange of sodium (Na⁺) and calcium (Ca²⁺) ions from the glass with hydrogen ions (H⁺) present in bodily fluids. This ionic interchange promotes the development of silanol (Si–OH) groups on the material’s surface 51.
Bioglass serves as a highly effective bone graft substitute in maxillofacial surgery due to its osteoconductive and osteostimulatory properties 52. After a tooth is extracted, the alveolar bone naturally resorbs, leading to a loss of bone volume. This can complicate or even prevent the placement of dental implants. Bioglass, often used in particulate form, is placed into the extraction socket to preserve the alveolar ridge. The bioactive properties of the glass promote the formation of new bone, maintaining the ridge's height and width for future prosthetic rehabilitation 53.
In restorative dentistry, bioactive glass is incorporated into various materials such as composites, liners, and adhesives to improve both functional and therapeutic properties. Its ability to release calcium and phosphate ions supports the remineralization of demineralized enamel and dentin, helping restore the mineral content of teeth. Additionally, the ion release raises local pH, creating an environment that inhibits the growth of cariogenic bacteria, thereby providing an antimicrobial effect. In cases of dentin hypersensitivity, bioactive glass helps by occluding exposed dentinal tubules, significantly reducing sensitivity and discomfort 54. Furthermore, when used in restorative materials, it can improve their mechanical integrity while offering long-term therapeutic advantages 55.
Periodontal Regeneration: Periodontics is a dental specialty dedicated to the prevention, diagnosis, and management of conditions affecting the tooth-supporting structures, collectively referred to as the periodontium 56. These include the gingiva (gums), alveolar bone, cementum, and periodontal ligament. Periodontists primarily address gingivitis which is a reversible gum inflammation and periodontitis, a chronic condition that can lead to permanent damage such as bone deterioration and tooth loss if not properly treated. Effective periodontic care is vital for preserving oral health and avoiding severe complications 57. In this domain, Bioglass is employed to repair periodontal defects by stimulating bone regeneration. When introduced to periodontal lesions, Bioglass particles react with bodily fluids, releasing sodium, calcium, and phosphate ions58. This ionic exchange initiates the formation of a silica gel layer on the particle surface, which is subsequently overlaid by a calcium-phosphate-rich phase. This layer crystallises into hydroxycarbonate apatite (HCA), a compound structurally similar to natural bone mineral. The HCA coating supports osteoblast attachment and proliferation, thereby enhancing bone growth and facilitating periodontal tissue regeneration 59.
Dental implantology is a specialized field focused on the surgical placement, restoration, and long-term maintenance of dental implants. A dental implant is a biocompatible medical device that is surgically positioned in the jawbone to replace a natural tooth root. This implant provides a stable foundation for prosthetic teeth, such as crowns, bridges, or dentures, effectively restoring both function and aesthetics for patients with missing teeth 60.
The bioactive surface of Bioglass-coated implants encourages the formation of a strong bond between the implant and the surrounding bone tissue. Additionally, the antimicrobial properties of Bioglass help in minimizing the risk of peri-implant infections, contributing to the long-term success of dental implants. It also serves as a coating material to enhance osseointegration.The osteostimulative effect of Bioglass, characterized by its ability to stimulate osteoblast activity and bone matrix formation, further underscores its utility in implant dentistry 61.
The rising demand for robust implants, driven largely by an aging population and a surge in trauma cases, presents significant challenge and to overcome this the Bioglass has been doped with various elements like the zirconium dioxide (ZrO2) and magnetite. Studies indicate that doping of 45S5 Bioglass with Zirconium dioxide improves the activity and results in more durable and biocompatible implants 62.
Dental and Orthodontic Adhesives: In orthodontics, Bioglass is incorporated into adhesives and sealants to mitigate enamel demineralization, a common issue during fixed appliance therapy. The mechanism involves the release of calcium and phosphate ions as mentioned in the above mechanism that leads to the formation of aHCA layer on the enamel surface. This layer remineralizes early carious lesions and serves as a barrier against acid attacks. Studies have demonstrated that orthodontic adhesives enhanced with Bioglass nanoparticles exhibit superior remineralizing effects and antibacterial properties, especially when doped with strontium ions, which further promote apatite formation and inhibit bacterial growth 63.
Endodontic therapy, Bioglass is utilized in root canal sealers and fillers to improve sealing ability and promote periapical healing 64. It also exhibits antibacterial properties by elevating the local pH and releasing ions that disrupt bacterial cell walls, thereby reducing the risk of reinfection. The bioactive layer upon contact with body fluid is rich in silica that facilitates the adhesion and proliferation of osteoblasts, promoting bone regeneration and sealing of the root canal system 65.
Caries Prevention and Remineralisation: Bioglass possesses exceptional antimicrobial properties that are valuable in biomedical applications. Its action is mainly due to the release of ions like Na⁺, Ca²⁺, and PO₄³⁻ in physiological fluids, raising local pH and creating an alkaline environment that inhibits bacterial growth. This ionic release also alters osmotic pressure around microbial cells, causing dehydration and cell lysis 66. Furthermore, Bioglass can physically damage bacterial membranes, leading to cell death. Therefore, its activity is enhanced by doping with antimicrobial metal oxides such as zinc, cobalt, and copper, with combinations resulting in synergistic effects that can be up to 100 times more effective. Silver-doped Bioglass exhibited both bacteriostatic and rapid bactericidal activities. Furthermore, the porous structure of this biomaterial facilitates the controlled release of metal ions, allowing for a sustained delivery of the antibacterial agent to dental materials 67. Prevalence of various Enterococcus species have been reported in the oral cavity 68.
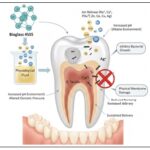
The antimicrobial activity of Bioglass reduces bacterial colonization, prevents infections, and promotes tissue healing thereby benefiting dentistry, orthopedics and wound care 69. A study reported that Bioglass 45S5 exhibited antimicrobial effects against E. faecalis using direct exposure test (DET) was used to evaluate the antimicrobial effect 70. The given Fig. 4, represents the antibacterial action of Bioglass in treating Dental caries 71.
FIG. 4: ANTI-BACTERIAL ACTION OF BIOGLASS IN TREATING DENTAL CARIES
Other Emerging Oral Health Applications: In orthodontics, Bioglass is incorporated into adhesives, sealants orthodontic brackets to mitigate enamel demineralization, a common issue during fixed appliance therapy 72. The mechanism involves the formation of HCA layer on the enamel surface. This layer remineralises early carious lesions and serves as a barrier against acid attacks.Studies have demonstrated that orthodontic adhesives enhanced with Bioglass nanoparticles exhibit superior remineralizing effects and antibacterial properties, especially when doped with strontium ions, which further promote apatite formation and inhibit bacterial growth 73.
Endodontic therapy, Bioglass is utilized in root canal sealers and fillers to improve sealing ability and promote periapical healing 63. It also exhibits antibacterial properties by elevating the local pH and releasing ions that disrupt bacterial cell walls, thereby reducing the risk of reinfection.
The bioactive layer upon contact with body fluid is rich in silica that facilitates the adhesion and proliferation of osteoblasts, promoting bone regeneration and sealing of the root canal system 74, 75, 76.
The given table 2 represents commercially available products of Bioglass.
TABLE 2: MARKETED PRODUCTS CONTAINING BIOGLASS
| Material | Composition and structure |
| PerioGlas® | Contains calcium, sodium, phosphate and silica; it is a granulated form of 45S5 Bioglass®. Particle size: 90–710 µm |
| Biogran® | Same composition as 45S5 Bioglass® (calcium, sodium, phosphate, and silica); particles of narrow size range. Particle size: 300–360 µm |
| BonAlive® | Special Bioglass (S53P4) consists of 53% SiO₂, 23% Na₂O, 20% CaO, and 4% P₂O₅ as weight percent. Particle size: 500–800 µm |
| NovaMin® | Identical with 45S5 Bioglass®, contains only calcium, sodium, phosphate, and silica in an amorphous matrix. Particle size: 18 µm |
Doping of Bioglass with Other Chemicals/ Herbs: Bioglass is often enhanced with herbal extracts to improve its properties for medical applications. This doping increases antimicrobial activity, aiding in infection prevention during bone and dental repairs. The natural compounds in herbs promote healing and tissue regeneration, creating a synergistic effect that boosts the performance of Bioglass. This combination offers a holistic approach that utilises both Bioglass and the benefits of medicinal plants. Bioglass has been infused with various metals such as cobalt, zinc, and silver, which provides advantageous properties of these metal ions in addition to the benefits offered by the Bioglass itself 77.
Herbs can be integrated into Bioglass to have combined benefits of the Bioglass and phytoconstituents present in the herbs 78. Bioglass can be doped with various potent herb extracts to have synergistic action, multi-functionality, controlled release and improved biocompatibility and therefore increasing their effectiveness in treating dental conditions and effective against Streptococcus mutans strains 79. The process of incorporating herbs into Bioglass majorly depends on the nature of the herb-extract, crude powder, purified compound etc. Various methods employed for the same are loading into porous Bioglass, surface coating, and direct incorporation during synthesis, etc. Herbs that have well documented oral benefits and that can be potentially combined with Bioglass include- Green tea, Red Clover, Turmeric, Neem, Liquorice, Chamomile, Aloe vera, Miswak, etc 80. Studies have reported that Bioglass doped with curcumin showed promising wound healing activity. Curcumin enhances the anti-inflammatory and antimicrobial effects, making this combination a promising option for improving tissue regeneration and reducing infection risks in wound care 81. Research has shown that Bioglass infused with Boswellia sacra extract exhibits antibacterial properties and promotes tissue healing and regeneration 82.
The future of Bioglass infused with herbs for oral health can offer innovative possibilities for treatment. One significant advancement is the creation of customized therapies, such as 3D-printed Bioglass-herb composite scaffolds that can be tailored to the unique anatomy of individual patients and their specific disease conditions 83. Additionally, targeted drug delivery systems could be developed, allowing these Bioglass-herb combinations to release therapeutic compounds in response to specific triggers, such as pH changes in inflamed tissues or during the production of acid by bacteria. Another potential application is in the prevention of peri-implantitis, which is a significant cause of dental implant failure 84. Herb-doped Bioglass coatings on dental implants could be designed to create surfaces that actively prevent the formation of biofilms and reduce inflammation around the implants. Furthermore, these Bioglass-herb composites might be utilized in regenerative endodontics to help rejuvenate damaged pulp tissue and encourage the regeneration of dentin. Recent advancements in the use of Bioglass include the addition of quercetin, which helps reduce oxidative stress and consequently diminish periodontal bone defects through various molecular mechanisms 85.
Bioglass in Other Fields: In Orthopedics, Bioglass and other biomaterials have played a significant role in bone repair for more than 30 years. Their effectiveness is largely attributed to their versatile properties, which can be modified to enhance biological responses 86. For instance, Bioglass can facilitate new bone tissue, enhancing the healing process, and even provide antibacterial effects 25. When the Bioglasscomes in contact with physiological fluid, it forms aHCA layer it releases ions like Ca2+, Si4+, Na+, PO43- which directly influence cellular signalling and promote bone regeneration 26. Bioglass enhances proliferation of osteoprogenitor cells, regulates gene expression and promotes angiogenesis which is critical for delivering nutrients and oxygen essential for bone healing 87.
The therapeutic effectiveness of Bioglass in Wound Healing is initiated by its dissolution in physiological fluids, which releases a variety of beneficial ions like calcium (Ca2+), silicon (Si4+), and phosphorus (P2O5). This ion exchange mechanism leads to a local increase in pH, creating an alkaline microenvironment that is detrimental to bacterial proliferation, thereby offering an inherent antibacterial effect 88. The released ions also modulate cellular behavior, promoting the migration and proliferation of key cells such as fibroblasts and keratinocytes that are vital for tissue regeneration. Furthermore, Bioglass has been shown to induce angiogenesis, the formation of new blood vessels, which is critical for supplying the wound with essential nutrients and oxygen 89. By regulating the inflammatory phase and promoting the proliferative and remodeling phases, Bioglass facilitates the deposition of new collagen and the formation of organized tissue, ultimately leading to accelerated wound closure with reduced scarring, making it a powerful tool for managing both acute and chronic wounds 90.
Bioglass also plays a significant role in the management of chronic and diabetic ulcers by enhancing wound healing and improving the quality of regenerated tissue 91. Its therapeutic effect is driven by the release of bioactive ions, which stimulate angiogenesis that is the process of development of new blood vessels and this helps to regulate the inflammatory response by encouraging the activity of anti-inflammatory macrophages 92, 93. Emerging application of Bioglass, includes its application in cosmetic and cosmeceutical fields. The patent underscores the incorporation of Bioglass into topical formulations that aim at enhancing skin appearance, particularly in reducing fine lines and improving texture. When applied topically, Bioglass particles interact with moisture on the skin, initiating an ion exchange that leads to the formation of a hydroxycarbonate apatite-like layer. This biomimetic process not only supports skin regeneration but also contributes to a smoother, more hydrated surface.
Challenges and Future Perspectives: Despite the significant bioactivity and compatibility of Bioglass, it faces several challenges that limit its widespread clinical and industrial application. One of the major challenges faced is its mechanical fragility. Traditional Bioglass compositions, such as 45S5, exhibit poor tensile strength and brittleness, making them unsuitable for load-bearing applications like orthopedic implants 94. Researchers have attempted to overcome this by developing composites or incorporating reinforcing agents, but achieving a balance between bioactivity and mechanical integrity remains complex. Another significant challenge lies in the processing and fabrication of Bioglass-based materials. The high melting temperatures and sensitivity to crystallization during sintering complicate the manufacturing of porous scaffolds and injectable formulations. Also, Rapid dissolution can lead to local pH changes and cytotoxicity, while slow degradation may hinder integration with host tissue 95.
From a clinical perspective, regulatory approval and translational hurdles also pose barriers. The variability in composition, particle size, and delivery methods across different formulations makes standardization difficult. Additionally, long-term in-vivo data on Bioglass performance, especially in soft tissue applications, is still limited. This affects clinician confidence and slows down broader adoption beyond dental and bone repair contexts 96.
Future prospectives: Bioglass is advancing rapidly with promising innovations. Nanocomposites combining Bioglass with polymers are improving strength and promoting remineralisation, with emerging self-healing variants that could extend restoration life. 3D and 4D printing technologies enable custom scaffolds for tissue regeneration, tailored to patient-specific defects. Bioglass-based bioinks in 3D bioprinting offer precise reconstruction of oral tissues with excellent biocompatibility 97. Additionally, Bioglass is being explored as a smart drug delivery system for antibiotics and growth factors, enhancing targeted therapy for dental conditions like peri-implantitis and periodontal regeneration 98. Injectable Bioglass is gaining momentum as a versatile material for regenerative therapies, offering minimally invasive solutions tailored to complex tissue defects. Future developments focus on enhancing its mechanical and biological performance through multifunctional composites, while also enabling controlled delivery of drugs and growth factors. Innovations like responsive formulations and stem cell integration aim to create dynamic, personalized treatments. With progress in customization and scalable production, injectable Bioglass is set to play a key role in dentistry, orthopedics, and soft tissue repair 99.
Clinical Trial Studies of Bioglass:
TABLE 3: CLINICAL TRIALS OF BIOGLASS
| NCT Number | Conditions | Study Status | Sex | Phases | Locations |
| NCT03786302 | Pulpotomy | Terminated | All | Phase2 | Faculty of Dentistry, 21512, Egypt |
| NCT04767243 | Chronic Periodontitis Bone Loss Intrabony Periodontal Defect | Completed | All | Phase4 | Department of Periodontology, 133207, India |
| NCT05049915 | Pseudoarthrosis of Bone | Unknown | All | Na | University Hospital Heidelberg, 69118, Germany |
| NCT05260853 | Invasive Ventilation Weaning | Unknown | All | Na | Thoraxklinik Heidelberg, 69120, Germany |
| NCT05974228 | Chronic Wound | Unknown | All | Na | NA |
| NCT03798184 | Self-etch Selective-etch Bioactive Glass Direct Resin Composite | Unknown | All | Na | University of Valencia, Spain |
| NCT05484492 | Alveolar Bone Resorption | Recruiting | All | Phase4 | University of Louisville, 40202, United States |
| NCT02982681 | Periodontal Diseases Bone Resorption | Completed | All | Phase3 | NA |
| NCT01878084 | Bone Loss Vertical Alveolar Bone Loss Horizontal Alveolar Bone Loss | Completed | All | Na | Tissue Engineering Laboratories, Egypt |
| NCT02316080 | Dentin Hypersensitivity | Completed | All | Phase4 | University of Sao Paulo, 14040904, Brazil |
Patents Related to Bioglass:
TABLE 4: DIFFERENT PATENT RELATED TO BIOGLASS
| Title | Link |
| Bioglass fermentation cylinder | https://patents.google.com/patent/CN222119207U/en |
| A surface-modified bioactive glass tooth desensitizer and its preparation method and application | https://patents.google.com/patent/CN119385842A/en |
| A plant-based bioactive glass and its application in oral care products | https://patents.google.com/patent/CN119302878A/en |
| Sponge comprising a recombinant collagen-like peptide (clp) and bioactive glass | https://patents.google.com/patent/WO2025016819A1/en |
| Stable bioactive glass formulations | https://patents.google.com/patent/US20240366482A1/en |
| Bletilla polysaccharide-mesoporous bioactive glass-gelatin hydrogel and application thereof | https://patents.google.com/patent/CN117771428A/en |
| A bioactive glass composite hydrogel scaffold material and its preparation method and application | https://patents.google.com/patent/CN116099041B/en |
| Storage device for Bioglass toothpaste | https://patents.google.com/patent/CN218594919U/en |
| Bioactive borated glass with addition of phosphorus pentoxide | https://patents.google.com/patent/BR102022019645A2/en |
| Micro-nano Bioglass restoration toothpaste and preparation process thereof | https://patents.google.com/patent/CN114557895A/en |
| Method for preparing Bioglass powder with different particle sizes in batch | https://patents.google.com/patent/CN110818270A/en |
| The preparation method of porous Bioglass dressing | https://patents.google.com/patent/CN106474535A/en |
| Mesoporous silica-loaded Bioglass composite material | https://patents.google.com/patent/CN106038333B/en |
| Bioglassfiber dental implant | https://patents.google.com/patent/KR101603474B1/en |
| Bioglass granular material and preparation technique thereof | https://patents.google.com/patent/CN104724922A/en |
| 1. System and kit for delivering collagen Bioglass composite bone grafting materials for regenerating hard tissues | https://patents.google.com/patent/US20150105748A1/en |
| Development, production and use of generic Bioglass, and its crystallized version, using napo3 as the exclusive source of phosphorus | https://patents.google.com/patent/BRPI0900608A2/en |
| Degradable mechanically enhanced Bioglass-based porous composite material and preparation method thereof | https://patents.google.com/patent/CN101288780B/en |
| Silver-containing, sol-gel derived Bioglass compositions | https://patents.google.com/patent/WO2000076486A1/en |
| Fluoride-containing Bioglassâ ¢ compositions | https://patents.google.com/patent/US4775646A/en |
ACKNOWLEDGEMENT: We would like to thank Dr. S.S. Kadam, Chancellor, Bharati Vidyapeeth (Deemed to be University), Dr. A. P. Pawar, Principal, BVDU Poona College of Pharmacy for providing the necessary facilities and support.
Funding: This article did not receive any specific grant from funding agencies.
CONFLICT OF INTEREST: The authors declare no conflict of interest.
REFERENCES:
- Dolejsova M: The impact of oral health on overall well-being: A comprehensive review. J Clin Dent Trials 2024; 8(1): 188.
- WHO releases Global strategy and action plan on oral health. Accessed September 10, 2025. https://www.who.int/news/item/26-05-2024-who-releases-global-strategy-and-action-plan-on-oral-health
- Mishra P: Social determinants of oral health: a comprehensive review of socioeconomic and environmental factors. Journal of Dental Care 2024; 1(1): 1-10.
- Tavares M, LindefjeldCalabi KA and San Martin L: Systemic diseases and oral health. Dent Clin North Am. 2014; 58(4):797-814. doi:10.1016/j.cden.2014.07.005
- Kisely S, Sawyer E, Siskind D, Lalloo R: The oral health of people with anxiety and depressive disorders - a systematic review and meta-analysis. J Affect Disord 2016; 200: 119-132.
- Hartnett E, Haber J, Krainovich-Miller B, Bella A, Vasilyeva A and Lange Kessler J: Oral Health in Pregnancy. JOGNN - Journal of Obstetric, Gynecologic, and Neonatal Nursing 2016; 45(4): 565-573.
- Skallevold HE, Rokaya D, Khurshid Z and Zafar MS: Bioactive glass applications in dentistry. Int J Mol Sci 2019; 20(23).
- Krishnan V and Lakshmi T: Bioglass: A novel biocompatible innovation. J Adv Pharm Technol Res 2013; 4(2): 78.
- Cao W and Hench LL: Bioactive materials. Ceram Int. 1996; 22(6): 493-507.
- Nowotnick AG, Xi Z and Jin Z: Antimicrobial biomaterials based on physical and physicochemical action. Adv Healthc Mater 2024; 13(32).
- Fernandes HR, Gaddam A, Rebelo A, Brazete D, Stan GE and Ferreira JMF: Bioactive glasses and glass-ceramics for healthcare applications in bone regeneration and tissue engineering. Materials (Basel) 2018; 11(12).
- Thrivikraman G, Athirasala A, Twohig C, Boda SK and Bertassoni LE: Biomaterials for craniofacial bone regeneration. Dent Clin North Am 2017; 61(4): 835-856.
- Lee BS, Tsai HY, Tsai YL, Lan WH and Lin CP: In-vitro study of DP-Bioglass paste for treatment of dentin hypersensitivity. Dent Mater J 2005; 24(4): 562-569.
- Hench LL: The story of Bioglass®. J Mater Sci Mater Med 2006; 17(11): 967-978.
- Rae T: The toxicity of metals used in orthopaedic prostheses. An experimental study using cultured human synovial fibroblasts. J Bone Joint Surg Br 1981; 63-(3): 435-440.
- Krishnan V and Lakshmi T: Bioglass: A novel biocompatible innovation. J Adv Pharm Technol Res 2013; 4(2): 78.
- Montazerian M and Dutra Zanotto E: History and trends of bioactive glass-ceramics. J Biomed Mater Res A 2016; 104(5): 1231-1249.
- Cao W and Hench LL: Bioactive materials. Ceram Int 1996; 22(6): 493-507.
- Cannio M, Bellucci D, Roether JA, Boccaccini DN and Cannillo V: Bioactive glass applications: a literature review of human clinical trials. Materials 2021; 14(18): 5440.
- Shearer A, Montazerian M, Sly JJ, Hill RG and Mauro JC: Trends and perspectives on the commercialization of bioactive glasses. Acta Biomater 2023; 160:14-31.
- Montazerian M and Dutra Zanotto E: History and trends of bioactive glass-ceramics. J Biomed Mater Res A 2016; 104(5): 1231-1249.
- Cichos S, Schätzlein E and Wiesmann-Imilowski N: A new 3D-printed polylactic acid-Bioglass composite for bone tissue engineering induces angiogenesis in vitro and in ovo. Int J Bioprint 2023; 9(5).
- Jose SC: Bioactive glass material and its applications in dentistry. Accessed September 11, 2025. www.dentaljournal.in
- Pawar V and Shinde V: Bioglass and hybrid bioactive material: A review on the fabrication, therapeutic potential and applications in wound healing. Hybrid Advances Elsevier B.V. 2024; 6.
- Fernandes JS, Gentile P, Pires RA, Reis RL and Hatton PV: Multifunctional bioactive glass and glass-ceramic biomaterials with antibacterial properties for repair and regeneration of bone tissue. Acta Biomater 2017; 59: 2-11.
- Varanasi VG, Owyoung JB, Saiz E, Marshall SJ, Marshall GW and Loomer PM: The ionic products of bioactive glass particle dissolution enhance periodontal ligament fibroblast osteocalcin expression and enhance early mineralized tissue development. J Biomed Mater Res A 2011; 98(2): 177-184.
- Xu YT, Wu Q, Chen YM, Smales RJ, Shi SY and Wang MT: Antimicrobial effects of a bioactive glass combined with fluoride or triclosan on Streptococcus mutans biofilm. Arch Oral Biol 2015; 60(7): 1059-1065.
- Allan I, Newman H and Wilson M: Antibacterial activity of particulate Bioglass against supra- and subgingival bacteria. Biomaterials 2001; 22(12): 1683-1687.
- Moghanian A, Firoozi S, Tahriri M and Sedghi A: A comparative study on the in-vitro formation of hydroxyapatite, cytotoxicity and antibacterial activity of 58S bioactive glass substituted by Li and Sr. Mater Sci Eng C Mater Biol Appl 2018; 91: 349-360.
- Ullah R, Zafar MS and Shahani N: Potential fluoride toxicity from oral medicaments: A review. Iran J Basic Med Sci 2017; 20(8): 841-848.
- Johnston NR and Strobel SA: Principles of fluoride toxicity and the cellular response: a review. Arch Toxicol 2020; 94(4): 1051-1069.
- Kirtana A and Seetharaman B: Comprehending the Role of Endocrine Disruptors in Inducing Epigenetic Toxicity. EndocrMetab Immune Disord Drug Targets 2022; 22(11): 1059-1072.
- Anil S, H.S.A. Alyafei S, Kitty George A and Paul Chalisserry E: Adverse effects of medications on periodontal tissues. Oral Dis Published Online May 13, 2020.
- Haps S, Slot DE, Berchier CE and Van der Weijden GA: The effect of cetylpyridinium chloride-containing mouth rinses as adjuncts to toothbrushing on plaque and parameters of gingival inflammation: a systematic review. Int J Dent Hyg 2008; 6(4):290-303.
- Tartaglia GM, Tadakamadla SK, Connelly ST, Sforza C and Martín C: Adverse events associated with home use of mouthrinses: a systematic review. Ther Adv Drug Saf 2019; 10: 2042098619854881.
- Poppolo Deus F and Ouanounou A: Chlorhexidine in Dentistry: Pharmacology, Uses, and Adverse Effects. Int Dent J 2022; 72(3): 269-277.
- Skallevold HE, Rokaya D, Khurshid Z and Zafar MS: Bioactive Glass Applications in Dentistry. Int J Mol Sci 2019; 20(23).
- Jafari N, Habashi MS, Hashemi A, Shirazi R, Tanideh N, Tamadon A: Application of bioactive glasses in various dental fields. Published online 2021.
- Ergucu Z, Yoruk I, Erdoğan A, Boyacıoğlu H, Hill R and Baysan A: The use of toothpastes containing different formulations of fluoride and bioglass on bleached enamel. Materials (Basel) 2023; 16(4).
- Shaikh MS, Fareed MA and Zafar MS: Bioactive Glass Applications in Different Periodontal Lesions: A Narrative Review. Coatings 2023; 13(4):716.
- Profeta AC and Prucher GM: Bioactive-glass in periodontal surgery and implant dentistry. Dent Mater J 2015; 34(5): 559-571.
- de Oliveira Roma FRV, de Oliveira TJL, Bauer J and Firoozmand LM: Resin-modified glass ionomer enriched with BIOGLASS: Ion-release, bioactivity and antibacterial effect. J Biomed Mater Res B Appl Biomater 2023; 111(4): 903-911.
- Al-Haddad A, Alarami N, Alshammari AF and Madfa AA: Efficacy of bioactive glass-based desensitizer compared to other desensitizing agents or techniques in dentin hypersensitivity: a systematic review. BMC Oral Health 2025; 25(1): 1-13.
- Lee BS, Kang SH, Wang YL, Lin FH and Lin CP: In-vitro study of dentinal tubule occlusion with sol-gel DP-Bioglass for treatment of dentin hypersensitivity. Dent Mater J 2007; 26(1): 52-61.
- Lynch E, Brauer DS, Karpukhina N, Gillam DG and Hill RG: Multi-component bioactive glasses of varying fluoride content for treating dentin hypersensitivity. Dental Materials 2012; 28(2): 168-178.
- Tang M, Ge M and Zhang X: Gelatin-Modified Bioactive Glass for Treatment of Dentin Hypersensitivity. Int J Mol Sci 2024; 25(22): 11867.
- Kumar A, Singh S, Thumar G and Mengji A: Bioactive Glass Nanoparticles (NovaMin®) for Applications in Dentistry. IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN. 2015; 14(8): 30-35.
- Chiang YC, Wang YC, Kung JC and Shih CJ: Antibacterial silver-containing mesoporous Bioglass as a dentin remineralization agent in a microorganism-challenged environment. J Dent 2021; 106: 103563.
- Kung JC, Wang WH and Chiang YC: The antibacterial and remineralization effect of silver-containing mesoporous bioactive glass sealing and Er-YAG Laser on dentinal tubules treated in a Streptococcus mutans cultivated environment. Pharmaceuticals 2021; 14(11): 1124.
- Profeta AC: Emerging developments in the use of bioactive glass for reconstruction of craniofacial bone. Br J Oral Maxillofac Surg 2015; 53(8): 760-762.
- Profeta AC and Huppa C: Bioactive-Glass in Oral and Maxillofacial Surgery. Craniomaxillofacial Trauma & Reconstruction 2016; 9(1): 1-14.
- Yadav P, Thomas S and Dutt Pathak A: Comparative evaluation of bioactive glass and xenograft with platelet rich fibrin for bony defects-an experimental and prospective clinical study. IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN. 2023; 22: 9-19.
- Alveolar ridge preservation using a bioactive glass particulate graft in extraction site defects - PubMed. Accessed September 19, 2025. https://pubmed.ncbi.nlm.nih.gov/12029801/
- SE S, AM D, Naik VM and Khanum Z: Recent Advances in Bone Grafts in Oral and Maxillofacial Surgery 2403; 6(3).
- Belluz M and Longhi EV: Periodontal Disease. Managing Psychosexual Consequences in Chronic Diseases. Published online 2025; 329-336.
- Nicholson JW: Periodontal therapy using bioactive glasses: a review. Prosthesis 2022; 4(4): 648-663.
- Farano V, Maurin JC, Attik N, Jackson P, Grosgogeat B and Gritsch K: Sol-gel Bioglasses in dental and periodontal regeneration: A systematic review. J Biomed Mater Res B Appl Biomater 2019; 107(4): 1210-1227.
- Motta C, Cavagnetto D, Amoroso F, Baldi I and Mussano F: Bioactive glass for periodontal regeneration: a systematic review. BMC Oral Health 2023; 23(1).
- Addy LD: An introduction to dental implants. Br Dent J 2024; 236(10): 753-757.
- Shaikh MS, Fareed MA and Zafar MS: Bioactive glass applications in different periodontal lesions: a narrative review. Coatings 2023; 13(4): 716.
- Hammami I, Fernandes Graça MP and Gavinho SR: Influence of zirconium dioxide (ZrO2) and magnetite (Fe3O4) additions on the structural, electrical, and biological properties of Bioglass® for metal implant coatings. Front Bioeng Biotechnol 2025; 13: 1537856.
- Chaichana W, Insee K and Chanachai S: Physical/mechanical and antibacterial properties of orthodontic adhesives containing Sr-bioactive glass nanoparticles, calcium phosphate, and andrographolide. Sci Rep 2022; 12(1): 6635.
- Huang G, Liu SY, Wu JL, Qiu D and Dong YM: A novel bioactive glass-based root canal sealer in endodontics. J Dent Sci 2022; 17(1): 217-224.
- Chitra S, Mathew NK, Jayalakshmi S, Balakumar S, Rajeshkumar S and Ramya R: Strategies of Bioceramics, Bioactive Glasses in Endodontics: Future Perspectives of Restorative Dentistry. Biomed Res Int 2022; 2530156.
- Drago L, Toscano M and Bottagisio M: Recent Evidence on Bioactive Glass Antimicrobial and Antibiofilm Activity: A Mini-Review. Materials 2018; 11(2): 326.
- Balamurugan A, Balossier G and Laurent-Maquin D: An in-vitro biological and anti-bacterial study on a sol-gel derived silver-incorporated Bioglass system. Dent Mater 2008; 24(10): 1343-1351.
- Bang SJ, Jun SK and Kim YJ: Characterization of physical and biological properties of a caries-arresting liquid containing copper doped bioglass nanoparticles. Pharmaceutics 2022; 14(6).
- Komiyama EY, Lepesqueur LSS and Yassuda CG: Enterococcus species in the oral cavity: prevalence, virulence factors and antimicrobial susceptibility. PLoS One 2016; 11(9): 0163001.
- Drago L, Toscano M and Bottagisio M: Recent evidence on bioactive glass antimicrobial and antibiofilm activity: a mini-review. Materials 2018; 11(2): 326.
- Wong KW, Li YJ and Yang HC: Antimicrobial properties of bimetallic-containing mesoporous Bioglass against Enterococcus faecalis. J Dent Sci 2025; 20(1): 510-521.
- Correia BL, Gomes ATPC, Noites R, Ferreira JMF and Duarte AS: New and Efficient Bioactive Glass Compositions for Controlling Endodontic Pathogens. Nanomaterials 2022; 12(9): 1577.
- Sheikhi Z, Nouri A, Ahmadi F and Nourian A: The effect of adding bioglass 45s5 to orthodontic adhesive on the shear bond strength of metal orthodontic brackets: An In-vitro Study 2024; 19(2): 1164.
- Alamri A, Salloot Z, Alshaia A and Ibrahim MS: The Effect of Bioactive Glass-Enhanced Orthodontic Bonding Resins on Prevention of Demineralization: A Systematic Review. Molecules 2020; 25(11): 2495.
- Washio A, Morotomi T, Yoshii S and Kitamura C: Bioactive glass-based endodontic sealer as a promising root canal filling material without semisolid core materials. Materials 2019; 12(23): 3967.
- Fepiosandi RA, Wahjuningrum DA, Widjiastuti I, Pawar A and Mulyani I: Bioactive glass, a promising endodontics material: article review. bioactive glass, a promising endodontics material: Article Review 2024; 17(4): 1851-1855.
- Huang G, Liu SY, Wu JL, Qiu D and Dong YM: A novel bioactive glass-based root canal sealer in endodontics. J Dent Sci 2022; 17(1): 217-224.
- Qin X, Ji L and Zheng J: A general strategy for preparing porous metal-doped bioactive glass fibers. Mater Lett 2021; 290: 129509.
- Schuhladen K, Roether JA and Boccaccini AR: Bioactive glasses meet phytotherapeutics: The potential of natural herbal medicines to extend the functionality of bioactive glasses. Biomaterials. Elsevier Ltd 2019; 217.
- Jain I, Jain P, Bisht D, Sharma A, Srivastava B and Gupta N: Use of traditional Indian plants in the inhibition of caries-causing bacteria - Streptococcus mutans. Braz Dent J 2015; 26(2): 110-115.
- Abuzenada B, Pullishery F and Elnawawy M: Complementary and alternative medicines in oral health care: an integrative review. J Pharm Bioallied Sci 2021; 13(2): 892-897.
- Jebahi S, Saoudi M and Farhat L: Effect of novel curcumin-encapsulated chitosan-Bioglass drug on bone and skin repair after gamma radiation: experimental study on a Wistar rat model. Cell Biochem Funct 2015; 33(3): 150-159.
- Ilyas K, Singer L, Akhtar MA, Bourauel CP and Boccaccini AR: Boswellia sacra Extract-Loaded Mesoporous Bioactive Glass Nano Particles: Synthesis and Biological Effects. Pharmaceutics 2022; 14(1).
- Rajzer I, Kurowska A and Frankova J: 3D-Printed Polycaprolactone Implants Modified with Bioglass and Zn-Doped Bioglass. Materials (Basel) 2023; 16(3).
- Pazarçeviren AE, Tezcaner A and Evis Z: Multifunctional natural polymer-based metallic implant surface modifications. Biointerphases 2021; 16(2).
- Zhu H, Cai C and Yu Y: Quercetin-Loaded bioglass injectable hydrogel promotes m6a alteration of per1 to alleviate oxidative stress for periodontal bone defects. Adv Sci 2024; 11(29).
- Dos Reis-Prado AH, de Souza JR and de Sousa Trichês: Bioactive glasses for bone tissue engineering: a bibliometric study of the top 100-most cited papers. Odontology 2025; 113(2): 488-530.
- Bai L, Song P and Su J: Bioactive elements manipulate bone regeneration. Biomaterials Translational 2023; 4(4): 248.
- Nandhakumar M, Gosala R and Subramanian B: Invigorating chronic wound healing by nanocomposites composed with bioactive materials: a comprehensive review. Biotechnol Lett 2022; 44(11): 1243-1261.
- Ren Z, Tang S and Wang J: Bioactive Glasses: Advancing Skin Tissue Repair through Multifunctional Mechanisms and Innovations. Biomater Res 2025; 29.
- Zhang K, Chai B and Ji H: Bioglass promotes wound healing by inhibiting endothelial cell pyroptosis through regulation of the connexin 43/reactive oxygen species (ROS) signaling pathway. Lab Invest 2022; 102(1): 90-101.
- Wu C, Zhou Y, Xu M, Han P, Chen L, Chang J and Xiao Y: Copper-containing mesoporous bioactive glass scaffolds with multifunctional properties of angiogenesis capacity, osteostimulation and antibacterial activity. Materials Science and Engineering Mater Biol Appl 2018; 82: 279‑289.
- Ma AN, Gong N and Lu JM: Local protective effects of oral 45S5 bioactive glass on gastric ulcers in experimental animals. J Mater Sci Mater Med 2013; 24(3): 803-809.
- Paliwal P, Kumar AS, Tripathi H, Singh SP, Patne SCU and Krishnamurthy S: Pharmacological application of barium containing bioactive glass in gastro-duodenal ulcers. Materials Science and Engineering C 2018; 92: 424-434.
- Hench LL and Jones JR: Bioactive Glasses: Frontiers and Challenges. Front Bioeng Biotechnol 2015; 3(11): 194.
- Meskher H, Sharifianjazi F, Tavamaishvili K, Irandoost M, Nejadkoorki D and Makvandi P: Limitations, challenges and prospective solutions for bioactive glasses-based nanocomposites for dental applications: A critical review. J Dent 2024; 150: 105331.
- Cannio M, Bellucci D, Roether JA, Boccaccini DN and Cannillo V: Bioactive Glass applications: a literature review of human clinical trials. Materials 2021; 14(18): 5440.
- Yun Y, Kang H, Kim EC, Park S, Lee YS and Yun K: Fundamental Properties and Clinical Application of 3D-Printed Bioglass Porcelain Fused to Metal Dental Restoration. Int J Mol Sci 2023; 24(8).
- Thomas NG, Junior FG de S and Ninan N: Bioglass in dentistry: A comprehensive review of current applications and innovative frontiers. J Dent 2025; 162.
- Mîrț AL, Ficai D, Oprea OC, Vasilievici G and Ficai A: Current and Future Perspectives of Bioactive Glasses as Injectable Material. Nanomaterials 2024; 14(14):1196.
How to cite this article:
Dsilva R, Gachake A and Shinde V: Bioglass and herbal therapeutics: a revolutionary approach to enhancing oral health management. Int J Pharmacognosy 2026; 13(1): 152-65. doi link: http://dx.doi.org/10.13040/IJPSR.0975-8232.IJP.13(1).152-65.
This Journal licensed under a Creative Commons Attribution-Non-commercial-Share Alike 3.0 Unported License.
Article Information
2
152-165
980 KB
187
English
IJP
Riya Dsilva, Arti Gachake and Vaibhav Shinde *
Department of Pharmacognosy, Poona College of Pharmacy, Erandwane, Pune, Maharashtra, India.
vaibhavshinde847@gmail.com
14 February 2026
17 March 2026
20 March 2026
10.13040/IJPSR.0975-8232.IJP.13(3).152-65
31 March 2026