A REVIEW OF ETHNOMEDICINAL PLANTS AND THEIR TRADITIONAL USES FOR THE TREATMENT OF HEPATOBILIARY DISEASE BY DIFFERENT TRIBES OF NORTH-EAST INDIA
HTML Full TextA REVIEW OF ETHNOMEDICINAL PLANTS AND THEIR TRADITIONAL USES FOR THE TREATMENT OF HEPATOBILIARY DISEASE BY DIFFERENT TRIBES OF NORTH-EAST INDIA
Jyotirmoy Das * and Bapi Ray Sarkar
Department of Pharmaceutical Technology, University of North Bengal, Darjeeling, West Bengal, India.
ABSTRACT: The investigation reveals that the diverse tribes of North-East India use a variety of herbal medicinal herbs. The goal of ethnobotanical research is to benefit mankind as a whole, therefore, it is important to preserve traditional medicinal plant knowledge. The investigation was carried out by collecting local medicinal herbs in cooperation with local ethical experts. The etiology of liver and biliary diseases is intricate and multifactorial, and they often have several symptoms. The investigation of several medical targets is required to treat comparable ailments. Modern hepatobiliary ailments treatments are still unsuccessful, and side effects are usually severe. The study's primary goals center on the possibility of ethnobotanical investigation and the necessity of preserving and establishing traditional medicinal knowledge in order to make it more widely accessible and to use it for the good of mankind. Diseases of the hepato-biliary system offer a serious medical and societal problem as morbidity rates climb exponentially. The typical therapeutic plants used by the tribes, totaling 28 species, were investigated and cataloged. 56 factory species from 29 families were commonly used as medicines by the tribes of North-East India. The locals believed medicinal plants could treat diseases like diabetes, hepatobiliary illness, and cancer. The results of this research validated and verified those from earlier studies that showed traditional local healers had a thorough understanding of how to use different plant parts and medicinal plants for various illnesses and disease types. This investigation unquestionably demonstrates the significance of Piper beetle plants to the residential environments of these two cultures as an ethnomedical remedy. Its significant ethnomedicinal status may be explained by the fact that this species is consumed almost every day as part of their cultural activities. The outcomes of the current study may further concentrate on the importance of traditionally used medicinal herbs for various diseases. Most newly found plants have at least a few prominent medicinal qualities consistent with the majority of accepted theories. Drawing on this historical understanding of utilizing plants to heal various ailments and conditions may also be beneficial in prospective pharmaceutical and medical research projects that might result in breakthroughs.
Keywords: Ethnobotany, Traditional Medicine, Hepatobiliary disease, Pathophysiology, North-East India
INTRODUCTION: The term "ethnomedicine" refers to all aspects of a person's health, including all clinical and non-clinical activities that represent their unique health needs.
It also includes all of their Abilities, Skills, and techniques. It is more than just a privileged examination of the spectacular or typical manifestation of strange therapeutic practices and culturally specific disorders.
In other words, the methods used by traditional healers to cure patients' illnesses, which rely on indigenous medicine and a few ritualistic rituals, are mostly a product of culture. It encompasses the entire reach and distribution of wellbeing-related experience, discursive information, and practice throughout various human populations. It serves as a crucial framework for comprehending indigenous communities and their interactions with the natural world. With the use of the cultural and biological knowledge inherent to the disciplines of anthropology and biology, it is the documenting of the effects of certain behaviors and practices. Ethnomedicine is the study of sickness and Hepatobiliary disease from a traditional perspective. Ethnomedicinal plants are the primary source of new medication discovery and development from local herbal healers' traditional herbal technology approaches. For many years, Ethnobotanical research has substantially contributed to the creation of novel medicines. It may also be valuable for contemporary medical procedures 1.
Assam to the east, Bangladesh to the south, and Assam to the west define the State's borders. The Khasis, Jaintia, and Garos are the main ethnic groups in the State. Sankardeva's "Bhagavata Purana," published about 1500 A.D. and the first Indo-Aryan literary work to do so, is where the word "Khasi" is first used. The State contains a wealth of diverse and rich plant life that hasn't yet been fully used for economic purposes. Such economic exploitation might be quite beneficial for the nearby tribal farmers if done properly. The region has a remarkable potential for the or other scientifically proven medicinal plants due to its ideal agro-climatic conditions, suitable soil, and abundance of rainfall, which are the main determinants for the diverse varieties of vegetation ranging from tropical and subtropical to mild or close to calm.
Ethno-medicine is the traditional knowledge that ethnic groups draw from various socioeconomic data to treat various illnesses and issues using natural cures. (For instance, flora or wildlife). The verbal transmission of this sort of knowledge from one generation to the next is common. Given that new pharmaceuticals and medical technology have rendered ancient healing methods outdated, modern societies should not support them. To cure local diseases and illnesses, traditional medicine is fast regaining popularity in today's society. Plants may contain large quantities of physiologically active compounds with important medicinal properties. Medications to treat diabetes, depression, cancer, and other diseases. According to World Health Organization (WHO) estimates from 1978, more than 80% of the populace in all impoverished countries still relies on ethnomedicines for their essential medical needs 2. Almost 65% of the people in our nation, especially in rural regions, still rely on traditional medicine for their medical treatment. As a result, it has become imperative to preserve all traditional and indigenous knowledge held by tribal tribes in our country and throughout the globe before it is too late. Also, employing traditional medicines to cure illnesses and learning about traditional plants offer enormous promise as prospective sources of helpful medical medications that were previously accessible or otherwise unknown to the general public.
Natural plant products are the source of 50% of all contemporary therapeutic medications. Hence, this understanding of utilizing traditional plants to treat illnesses might also be a valuable source for future pharmaceutical research, perhaps leading to the development of life-altering medications or cancer treatments, among other things. Several tribal populations' ethnomedical practices and expertise have been uncovered through recent investigations in India 3. This particular study's goal is to learn more about the plants utilized by traditional healers in one of the wettest areas on Earth, North-East India,and to make an effort to determine the level of plant conservation in these two remarkable regions. Genetic resources, especially plant resources, are part of biological diversity.
They serve as the foundation for the ongoing evolution and upkeep of the life-supporting frameworks on the planet and promote the sustainable advancement of humankind's economy, science, technology, culture, and spirituality 4. In recent decades, both the interest in ethnomedicine and the sale of herbal products in local and international markets have increased. According to the World Health Organization, 80% of rural communities in developing nations rely mostly on herbal medicines to meet their essential medical requirements 5. In India, there are 45,000 officially recognized plant speciesand estimates place the number of medicinally significant plant species at 7,500 6. The use of ethnomedicinal herbs considerably impacts the lives of rural tribal Indians 7. Even now, the native populations that cohabit with the forests have managed to maintain a highly balanced level of mental and emotional well-being without endangering biodiversity. Arunachal Pradesh, the biggest State in North-Eastern India, has a long natural and cultural variety history. There are about 5,000 angiosperm species in the State, and 500–600 of these are allegedly employed in traditional ethnomedical procedures 8.
Further than 26 main tribes and 110sub-tribes, all of which have a rich history of Ethnobotanical knowledge, live in the state. Every one of these ethical gatherings has developed its collection of traditional knowledge handed down orally from generation to generation about their own religious and philosophical beliefs and their agrarian and ethnomedical practices. Nonetheless, owing to shy preservation, attestation, and creation sweats, these priceless traditional knowledge systems can come 9. During the last 20 times, numerous academics have worked to collect information on the ethnomedical practice published about 1500 A.D. and traditional medical styles used by Adi, else known as, Apatani, Galo, Idu Mishmi, Tangsa, and Wancho are only incompletely proven at this time 10. So, far little is known about the ethnomedical practices of several tribes and sub-tribes, including the Bugun (Khowa), Digaru Mishmi, Sherdukpen, and Zakhrings. The variety of ethnomedicinal plants, Hepatobiliary conditions treated, homegrown agreement, species, and family application values were all measured in this study.
Hepatobiliary Disease: A wide range of illnesses that affect the liver and biliary system are referred to as hepatobiliary diseases, including those brought on by neoplasia, toxic chemicals, alcohol use, poor nutrition, metabolic abnormalities, and heart failure 11.
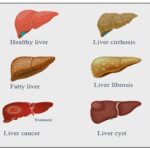
Hepatocellular carcinoma (HCC), gallbladder cancer, intrahepatic cholangitis-melanoma, and extrahepatic Cholangiocarcinoma are among the hepatobiliary cancer forms addressed by these recommendations. Any condition that affects the hepatobiliary system's capability to operate typi-cally is appertained to as hepatobiliary illness 12. The complaint may affect everyone from a simple infection or scars to life-changing ails like cancer. The liver, gallbladder, and corrosiveness tubes are the hepatobiliary system's organs. The identification sign of liver diseases are shown in Fig. 1. One of the body's major organs, the liver is located in the upper right corner of your belly 13. Some of the essential fleshly processes it carries out include:
- Bile juice production
- Glycogen is a sort of sugar storage.
- Cleaning hazardous toxins out of the blood
- Producing blood clotting-supporting proteins
A little organ located under the liver called the gallbladder holds corrosiveness, a fluid needed for the breakdown of fats 14. The corrosiveness conduit transports corrosive-ness from the gallbladder to the small intestine 15.
FIG. 1: IDENTIFICATION OF HEPATOBILIARY DISEASE
Types of Hepatobiliary Disease:
Choledocholithiasis: Gallstones in the corrosiveness conduit that have blocked it are known as Choledocholithiasis. The gallbladder and the corrosiveness conduit may develop gallstones, or the corrosiveness conduit itself might develop gallstones 16. Frequently, corrosiveness colors or cholesterol make up gallstones. Mariners of calcium and cholesterol make up fewer common gallstones 17. An overproduction of bilirubin, an orange-unheroic color, or cholesterol, an insufficiency in corrosiveness swab stashing, or infection 18, may cause the conformation of cholesterol or color monuments.
Primary Sclerosing Cholangitis: The bile duct narrows due to the liver illness’s primary sclerosing cholangitis. Bile builds up in the liver as the condition steadily worsens, harming the cells. Cirrhosis and liver failure may be brought on by the spread of scar tissue throughout the liver. Primary sclerosing cholangitis has no known origin but is linked to inflammatory conditions such as Crohn’s disease, ulcerative colitis, and inflammatory bowel disease 19.
Liver Cirrhosis: Due to excessive alcohol use or a viral infection, cirrhosis causes significant liver scarring and impaired liver function. National Institutes of Health (NIH) asserts that cirrhosis may occur in those who consistently use alcohol for over ten years. When the liver is exposed to hazardous substances for a long time, excessive scar tissue is formed, making it difficult for your liver to repair. In cirrhosis, the liver is stiff and restricted 20.
Autoimmune Liver Diseases: The immune system protects the body by battling and eliminating foreign invaders and toxic substances. However, in autoimmune liver illnesses, the body's immune system attacks the liver's organs (liver tissues and bile duct tissues), causing inflammation and damage to the liver. One instance is autoimmune hepatitis.
If left untreated, autoimmune liver disease can progress to liver disease, malignancy, and cirrhosis of the liver 21.
Fatty Liver Disease: An inordinate accumulation of liver fat results in an adipose liver complaint. Middle-aged persons are more likely to witness it. Hepatic steatosis is another name for adipose liver complaint. Two forms of adipose liver exist Non-alcoholic Adipose Liver Alcohol use isn't linked to the accumulation of fat in the liver. Alcoholic Adipose Liver Intemperance in alcohol is linked to a buildup of fat in the liver. The simple adipose liver is a milder form of adipose liver complaint that develops beforehand. The advanced form of non-alcoholic Steatohepatitis (NASH) damages liver cells and inflames the liver, leading to liver damage, liver cancer, swelling, and eventually failing the liver 22, 23.
Acalculous Cholecystography: Gallbladder abnormality, also known as Acalculous cholecystography or biliary dyskinesia is a motility disease system in which the gallbladder has poor corrosiveness drainage. The liver secretes corrosiveness, dark green to unheroic-brown fluid that's kept in the gallbladder. The sphincter of Oddi, a muscular stopcock, controls the passage of corrosiveness from the gallbladder to the small intestine (through the corrosiveness conduit). Corrosiveness may not flow typically, causing it to overflow into the gallbladder due to a sphincter of Oddi problem or a metabolic abnormality of the gallbladder 24.
Portal Hypertension: The portal venous system may experience elevated blood pressure due to liver cirrhosis. The portal vein, a significant vein that merges veins from the pancreas, spleen, intestine, stomach, and pancreas, further branches as it passes into the liver. Blood pressure elevation generates varies, which enlarges, bursts, and bleeds in the veins 25.
Jaundice: When bilirubin, a yellow pigment created by the liver's breakdown of RBC, builds up in our liver, a condition known as jaundice develops. A viral infection, clogged bile ducts, liver problems, or certain drugs may all contribute to this condition, which is marked by the yellow color of the skin and sclera, the white parts of the eyes 26.
Hepatitis: An inflammation in the liver tissue is known as hepatitis. Long-term exposure to drugs, alcohol, or other poisons may cause hepatitis. While it may sometimes happen as a result of an autoimmune reaction in which immune system antibodies (proteins) harm your liver tissue, viral infections are often to blame 27.
Gallbladder Cancer: An uncommon condition known as gallbladder cancer develops when healthy cells getirritations (DNA mutations) that cause them to proliferate uncontrolled and form tumors. Typically, cancer starts in the gallbladder's inner layers and spreads to the neighboring healthy tissues 28. It has four phases:
Stage I: Cancerous cells are restricted to the inner layers.
Stage II: Tumor has spread to the outer layers.
Stage III: Lymph nodes and adjacent organs have been affected by cancer.
Stage IV: Cancer has started to spread to the body's far-off organs.
Liver and Bile Duct Cancer: A tumor is a grouping of aberrant cells that may signal the start of liver cancer. Benign tumors do not metastasize or spread to surrounding tissues. Malignant tumors start to invade the tissues, lymph nodes, or organs in the area, impairing their functionality. Malignant liver malignancies predominate and may cause liver failure. A malignancy called Cholangiocarcinoma develops in the bile duct connective tissue 29.
Liver Failure: When a significant piece of your liver is damaged and unable to function, liver failure results in untreated cases of a variety of liver conditions that may result in liver failure and associated issues including cerebral edema, blood clotting issues, and kidney failure. The sole alternative is often a liver transplant, which is generally successful 30.
Treatment 31: Depending on the underlying reason, treatment options include:
- Giving up alcohol and tobacco use.
- Salt consumption is often reduced as part of diet adjustment.
- Dietary program (obese people).
- Lithotripsy for the treatment of gallstones.
- Drugs to treat symptoms of a viral infection and other conditions.
- Drugs to manage autoimmunity.
- Controlling diabetes and stress.
- Liver transplants in serious situations.
Prevention 32: It is possible to stop liver disease by:
- Vaccinations
- Managing diabetes.
- Eating well.
- Moderate alcohol consumption.
- Upkeep a healthy weight.
- Refraining from approaching an infected individual.
- Reducing exposure to hazardous substances.
Types of liver diseases and possible causes 33:
- Alcohol-related liver disease - consistent alcohol abuse.
- Non-alcoholic fatty liver disease - fat may accumulate in the liver as a result of obesity.
- Hepatitis - contracting a virus, often consuming too much alcohol.
- Hemochromatosis is a gene that runs in families and may be transferred from parents to children.
- Primary biliary cirrhosis - an immune system issue may be to blame for this condition.
Ayurvedic View: Liver diseases are classified in Ayurveda as YakritVikaraa. Vikara means disturbance or derangement, physical deformity, or ill State in Yakrit. According to Acharya Sushruta, the liver is produced from the blood at the embryonic stage. It is thought to be the primary location for blood. Even before bodily dissection and circulatory research in contemporary medicine, the Acharyas Charaka and Sushrutawere referred to 3000 years ago as the place of color responsible for bile variation (ranjaka pitta). Alcohol use, repressing desires that come naturally, consuming spicier and penetrating foods and drinks, heavy and blocking substances, resting during the day and waking up at night, any external harm to the liver, etc. are all potential causes of liver problems, according to Ayurveda. Ayurveda medicine uses carminative, digestive, laxative, and cholagogue herbs to treat liver diseases. Kapha and pitta-aggravated dosh may be expelled extremely effectively with panchakarma 34.
There are many Ayurveda medicines and preparations for liver diseases in North East:
- Bhomyamalaki
- Sharapunkha
- Kumari
- Bhringaraja
- Amalaki
- Draksha
- Guduchi
- Punarnava
- ArogyavardhiniVati.
- Rohitakarishta.
- Patolakaturohinyadikashaya.
- Avipattikarachoorna.
- Lohasavam.
- Punarnava mandur.
FIG. 2: COMMONLY USED MEDICINAL PLANTS WITH HEPATOPROTECTIVE PROPERTIES IN NORTH EAST INDIA 35
Many plants and mixtures have been suggested to have hepatoprotective properties Fig. 2. Beginning with Ayurveda medicine and expanding to the North East and other traditional medical systems, natural liver disease treatments have a long history. In order to support clinical efficacy, the strengths of traditional medical systems have been carefully combined with the contemporary ideas of evidence-based medical evaluation, standardization, and randomized placebo-controlled clinical trials, leading to a paradigm shift in favor of the therapeutic evaluation of herbal products in liver disease models 36. To get a comprehensive improvement, speak with the greatest Ayurveda physicians at Life Line Ayurvedic Herbal Clinic who believe in treating the patient as a complete. By administering medicines that balance the underlying dosha, we guarantee long-term results and efficient treatment for illnesses.
MATERIAL AND METHOD:
Study Sites:
Meghalaya: The exploration was conducted in the village of Sohra and Mawsynram, located in Meghalaya's East Khasi Hills District and is, independent. The agreements are around 56 and 60 kilometers. Nearly all of the population are from the Austro-Asian linguistic group's matrilineal Khasi and War groups. While they speak distinct dialects, these two groups share a great deal of the same artistic and traditional practices. Meghalaya's two locales with the most monthly downfall are Cherrapunjee (Sohra) and Mawsynram, with average periodicrains of 450 elevations and 467 elevations, independently. Agriculture will continue to be the crowd's major income source through 2019. For numerous individualities in these regions, other sources of income include the birth of limestone and the product of cement in cement manufactories. The limestone mining operations and cement plants have more significantly impacted the area's land, water, and timber. At Sohra (Cherrapunjee) and Mawsynram town lets, the goods on the terrain may be seen in the reduction of timber cover. Despite these fatal dislocations done in the name of development, these research regions maintain a large range of factory species and are home to colorful holy grooves in the State 37.
Tripura: The study was carried out in Tripua's North Tripura district, which has a geographical area of 1422.19 km2 and is situated at latitude 256.487 and longitude 845.230. The district has a total population of 422,370 and is split into Dharmanagar, Kanchanpur, and Panisagar subdistricts. Bengali, Tripuri, Halam, Reang, Chakma, Manipuri, and Debbarma are the principal ethnic groups in the districts, and they practice Hinduism, Christianity, and Buddhism 38.
Arunachal Pradesh: The study was conducted in the Changlang district of Arunachal Pradesh. The Changeling is home to the Tangsas tribe, which is the front between India and Burma. Singphos live on the banks of the Teang and Noa Diking rivers and reach into the Khamptis’ homeland to the southeast. The Apatami tribe lives in a valley of the lower Subansiri district's centere, close to the district office. There are 38,870 Monpas living in Tawang in the West Kameng district. The Adis are a group of tribes in the East, West, and upper Siang districts that mostly rely on the reserve forest plants for food and medicine. The Adis have a reputation for the medicinal traditions of the Padam clan. With the aid of indigenous guides, woodland exploration was carried out in various Arunachal Pradesh districts. For the investigation, standard plant-gathering techniques were used. The plant's leaves, and reproductive components-seeds, and were gathered, dried, and kept in a herbarium. The use of medicinal plants by the various tribes of Arunachal Pradesh was discussed with local medical specialists, village heads, and old people in order to obtain information. Plant identification was done in Shillong at the BSI, NEHU, and NEBRC 39.
Mizoram: The Indo-Burma and Himalayan biodiversity hotspots include a sizeable chunk of North East India (NE India). The 23rd State of the Indian Union is Mizoram, with a total area of 21,087 sq. km. It is located between Bangladesh and Myanmar (Burma). A significant state in Northeastern (NE) India, Mizoram is also one of the world's 25 mega-biodiversity hotspots. Mizoram's three types of woods are subtropical hill forests, tropical semi-evergreen forests, and tropical wet evergreen forests.
As a result, Mizoram has a variety of forest kinds that are extremely valuable to humanity. However, several human disturbances, including shifting agriculture, timber harvesting, the extraction of firewood by underprivileged/rural tribal people, industry, and in certain parts of the State, such as Aizawl, urbanization, affect these woodlands. In NE India, where the economy is primarily agrarian and rural, over 80% of the population is dependent on agriculture, about 27% of the population is tribal who live on subsistence, and almost 87 percent of the population lives in poverty in nearly 43,000 villages. According to the proposed classification, the vegetation of Mizoram is sub-tropical to montane sub-tropical in the high hills and tropical evergreen and semi-evergreen forests in the lower altitude hills. Tropical and semi-evergreen forests comprise a large component of Mizoram's forest cover. It is important to note that there are very few doctors and other medical professionals in Mizoram compared to the overall population (1:3415 for doctors). Moreover, Mizoram's geography is to blame for the underdeveloped communication infrastructure in the State. Because they cannot use contemporary medical techniques, people in rural areas look to nature for cures 40.
Manipur and Assam: Information on medicinal plants was acquired by performing a random survey in a specific district of Assam and Manipur. 84 plant species were identified using several workers' standard keys. The life sciences department's ecology, cytogenetics, and plant breeding laboratory has maintained the collected plant specimens for historical purposes. Each species includes its taxonomy, family, Assamese and Manipuri vernacular names, and the part(s) utilized in traditional medicine to treat illnesses. Information was gathered during a field survey through well-prepared questionnaires, interviews with knowledgeable community members, observations, and talks with traditional herbal healers 41.
Nagaland: The study was carried out in Khonoma village, which is located in Nagaland and has an elevation range of 1200m to 2868m above sea level and is a part of the Indo-Burma and Eastern Himalayan Biodiversity Hotspots. It was established 400 years ago by an Angami Naga tribe. There are 500 dwellings and 2500 people living in the village. The region experiences yearly rainfall of between 2000 and 2500 mm. Tropical semi-evergreen forests, moist deciduous forests, temperate broadleaf forests, gregarious pine forests, and secondary moist deciduous forests are among the several types of forests that may be found there (IIRS, 2003). The Khonoma people's primary activity is agriculture, and the dominant land use systems are wetland paddy cultivation and alder-based jhum (slash and burn). Additional sources of income include some government positions, piggery, basketry, carpentry, and other handicrafts. Non-timber forest products can be taken from the forest and used for a variety of domestic purposes, but they cannot be sold for profit. Khonoma village is well regarded for being a repository of conventional wisdom founded on reliable scientific foundations. Khonoma village recently succeeded in having hunting and logging prohibited in its extensive forest regions, which allowed for the restoration of its abundant natural resources and helped pave the way for the creation of the nation's first "Green village." In the current study, "medical herbs" refers to plants without woody components that have historically been utilized to cure various human illnesses and maladies.
Information was obtained on the traditional uses of wild and partially domesticated plant species that the Khonoma people have for medicinal purposes. This information includes family, seasonal availability, vernacular Angami and scientific names, mode of application identifying the plant components utilized, and sorts of diseases treated. The questionnaires were filled out based on in-person interviews with the respondents. Furthermore, interviewed were several of the village's traditional healers. After then, the information was cross-checked and examined. With the aid of regional field guides, plant specimens were collected, and herbaria were set up. The specimens were recognized with the assistance of professional advice, material that was already available, and references to herbaria from other institutions. To compile secondary data, books on medicinal plants and herbarium by various authors, organizations, and institutions underwent thorough reviews (Nagaland Bioresource) Mission 2009, Deorani and Sharma 2007. The herbariums were later placed in the NEHU Shillong Department of Environmental Studies 42.
Sikkim: The Himalayan region's abundant biodiversity is primarily explained by the presence of various geological, physiological, topographical, ecological, and climatic zones. The Indian State of Sikkim is situated between the latitudes of 27o4' 46'' and 28o7' 48'' N, the longitudes of 88o58' to 88o5' 25'',from 100 meters to 8598 meters above sea level is the Mighty Mt. Kanchenjunga. In addition to sharing borders with nations like China, Tibet, Nepal, and Bhutan Sikkim is closely related to the Siliguri corridor in West Bengal, India. Sikkim has 490 medicinal plants, which make up a large portion of the world's total number of medicinal plants. A few of Sikkim's medicinal species are also employed in Ayurvedic and pharmaceutical formulations on a commercial scale. All significant medicinal plants in Sikkim's Himalayan region must be known and preserved using an effective scientific method. The primary subject of this study is a group of significant medicinal plants indigenous to Sikkim's Himalayan area and thought to possess potent therapeutic potential. This will also be useful for researchers or scientists working on this subject in identifying different therapeutic compounds derived from this study's list of 51 medicinally significant plants from the Sikkim region of the Himalayas 43.
Collection of Data: The Ethno- medical information on a number of plants was recorded via surveying and canvassing the locals who had traditional knowledge. Traditional drug interpreters who primarily calculate on original requests and timber goods, senior individualities (progressed between 30 and 95), and those eager to conduct their traditional knowledge acquired via strain or previous guests all permanently dwell in the exploration locales. A thorough list of plants was kept, with information on their family, corridor employed, ails and diseases they were related with, composition, and cure. Images and proven samples were taken throughout the check to guarantee accurate and thorough species identification. With the application of former standard literature, like the foliage of Tripura, the Greenery of Assam, the Woods Verdure of Meghalaya, Manipur, Arunachal Pradesh, and many further vegetations, the identification of the licit scientific names was established. A portion of the sample was also put down at the Division of Herbal Wisdom at NEHU for unborn reference after the identification was latterly vindicated by BSI, Shillong, Meghalaya, and BSI Sikkim also.
Statistical Analysis: The data was arranged methodically and every species' botanical name, family, factors employed, and ethnomedical operations were listed below.
Informants’ Consensus Factor (FIC): The following formula was used to compute an informant's consensus factors in request to determine the homogeneity of the information obtained.
FIC=Nur- Nt / Nur -
Where, Nt= The quantity of species used to treat that specific classification by informants, Nur = the quantity of utilized announced in that classification of diseases by informants.
Fidelity Level (FL) Value: The Fidelity Level value calculation shown below was used to compute the proportion of informants who claimed to have used certain plants for the same primary purpose:
Fl (%) =Ip100/Iu
Where, Iu = The entire number of informants who adverted analogous plants for some diseases, while Ip = The volume of informants who independently suggested using a variety of plant species for a single sickness.
RESULTS AND DISCUSSION: Throughout the course of this discourse, 110 species from 56 families and 92 rubrics have been identified. The tribal people employ the greatest variety of locally accessible medicinal plant species. After the usage of fruits, roots, entire plants, seeds, tubers, bark, etc. by the tribal individuals of these two villages, it was discovered that leaves are the medicinal plant components they most commonly utilize to treat different maladies and diseases. Before they were made safe for use and eating, these plant components underwent many stages of processing. Others were consumed raw or taken as a decoction orally, while others were turned into a paste and used topically. It should be emphasized that many medicinal plants were blended with various other plants or plant parts and other chemicals, such as lime, before being used.
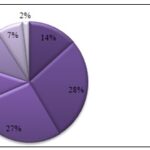
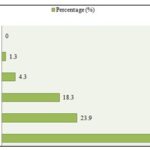
According to widespread conventional wisdom, the combination improves the medicine's therapeutic benefits and potency. Traditional medicines and traditional knowledge of plants can be used to treat different Hepatobiliary diseases, ailments, and injuries ranging from minor cerebral pains, hacks, and contagious infections to significant ones like epilepsy, paralysis, jaundice, menorrhagia, hypertension, tumors, diarrhea, food poisoning, and rheumatism. Out of the 110 species discovered, it has been determined that 51 of them are wild plants found in nearby grasslands or forests, and just 19 species are developed by tribal individuals as alternative food sources, as kinds of revenue, or for their medicinal worth. In addition, divided among 92 genera and 56 families, are dicots, while 18 are monocots, 2 are Gymnosperms, and 1 is a pteridophyte. During the field visits, 230 informants (140 male and 90 female) between the ages of 30-95 were questioned from 40 different homes Table 1 Fig. 3. They have a literacy rate of 52.2%, a primary education rate of 23.9%, a secondary education rate of 18.3%, a higher secondary education rate of 4.3%, and a college degree rate of 1.3% Table 2, Fig. 4.
TABLE 1: DISTRIBUTION OF TRADITIONAL INFORMANTS' AGES AND GENDERS
| Age groups | Gender | Total respondents | Percentage (%) | |
| Male | Female | |||
| 30 - 40 | 17 | 14 | 31 | 13.5 |
| 41 - 50 | 36 | 28 | 64 | 27.8 |
| 51 - 60 | 45 | 18 | 63 | 27.3 |
| 61 - 70 | 13 | 13 | 26 | 11.3 |
| 71 - 80 | 16 | 9 | 25 | 10.8 |
| 81 - 90 | 11 | 6 | 17 | 7.4 |
| 90> | 2 | 2 | 4 | 1.9 |
| Total | 140 | 90 | 230 | 100 |
FIG. 3: AGE CHART OF TRADITIONAL INFORMANTS
FIG. 4: INFORMANTS’ EDUCATIONAL LEVEL
TABLE 2: INFORMANTS’ EDUCATIONAL LEVEL
| Educational level | Number of individuals | Percentage (%) |
| Illiterate | 120 | 52.2 |
| Primary | 55 | 23.9 |
| Secondary | 42 | 18.3 |
| Higher Secondary | 10 | 4.3 |
| College | 3 | 1.3 |
| University | - | - |
| Total | 230 | 100 |
The Informant’s Consensus Factor (FIC) was loftiest for the order of Hepatobiliary conditions (1.80) and smallest for the group in the order of Other Affections conditions (0.16) Table 3. Low FIC and incitement for those affections gathered under the" others" class indicate that the informants do not appear to concur with each other over applying a particular factory species. High FIC and incitement for pneumonic conditions indicate that a couple of factory species had been accounted for to be employed for its treatment. Also, the Fidelity Level score ranged from least (39.65) for the Asparagus racemosus group under the gastrointestinal diseases order to loftiest (78.88) for the Piper insect bunch under the outside detriment and bleeding problems order Table 4.
TABLE 3: DISEASE TYPE, INFORMANT'S CONSENSUS FACTOR
| Ailments/Diseases category | Reported uses (Nur) | Number of taxa (Nt) | Informant’s consensus factor (FIC) |
| Antidote | 8 | 5 | 1.03 |
| Blood-related diseases | 4 | 3 | 1.04 |
| Cardiovascular diseases | 22 | 7 | 1.26 |
| Dermatological, fungal and bacterial infection | 25 | 20 | 1.05 |
| External injury and bleeding | 56 | 13 | 1.15 |
| Gastrointestinal | 69 | 56 | 1.62 |
| Musculoskeletal and bone fracture | 49 | 18 | 1.05 |
| Oral Dental and ENT | 30 | 9 | 1.45 |
| Hepatobiliary diseases | 8 | 3 | 1.80 |
| Urinogenital diseases | 15 | 5 | 1.3 |
| Neurological diseases | 6 | 2 | 1.2 |
| Respiratory ailments | 27 | 15 | 1.5 |
| Others | 55 | 40 | 1.4 |
TABLE 4: FIDELITY LEVEL FOR THE MOST WIDELY USED MEDICINAL HERBS
| Medicinal Plants | Ailments/Diseases Category | Ip | Iu | FL (%) |
| Agapetesvariegata | Gastrointestinal | 8 | 12 | 78.88 |
| Ageratum conyzoides | Outside injury and bleeding | 10 | 19 | 52 |
| Aloe Vera | Dermatological, contagious, and bacterial infections | 18 | 25 | 71.23 |
| Asparagus racemosus | Gastrointestinal | 6 | 14 | 39.65 |
| Centella asiatica | Blood-related diseases and Gastrointestinal | 12 | 26 | 45 |
| Cinnamomum tamala | Oral Dental and ENT and Gastrointestinal | 18 | 33 | 58.36 |
| Citrus macroptera | Others (fever) | 56 | 73 | 75.23 |
| Citrus medica | Others (Cough and cold) | 56 | 74 | 55.21 |
| Eupatorium adenophorum | External injury and bleeding | 14 | 22 | 53.21 |
| Fagopyrum esculentum | Cardiovascular, Others (Diabetes), and outside injury and bleeding | 12 | 23 | 51.20 |
| Piper beetle | External injury and bleeding | 15 | 17 | 78.88 |
Using this information, they created crude Phyto-medicinal extracts to treat various illnesses, from basic ones like the common cold to more complex ones like diabetes and cancer. These conventional herbal treatments are almost invariably linked to conventional prayers, rituals, and beliefs. Before being administered for the treatment of different Hepatobiliary diseases, medical treatments are often always sanctified utilizing ancient beliefs and rituals. The current research results supported and confirmed findings from past studies indicating traditional local healers had extensive knowledge of how to employ various plant parts and medicinal plants for various diseases and diseases. The fact that this species is eaten virtually daily as part of their cultural activities combined with the Areca nut may account for its high ethnomedicinal status. The tribal residents of these seven states’ residents appear to come up short on information, mindfulness, and ethnomedicinal abilities fundamental for treating pneumonic disorders, despite informants mentioning few plants throughout this investigation. For tribal people residing in mountainous regions like the Northeast, hepatobiliary illness is also a serious health concern. The northeast is home to various plants that are particularly significant for hepatobiliary illness. The gathered information is shown in the tables Ethnomedicinal plants used for the treatment of hepatobiliary disease in Arunachal Pradesh Table 5, Assam and Manipur Table 6, Nagaland Table 7, Mizoram Table 8, Meghalaya Table 9), Tripura Table 10, Sikkim Table 11. The tables provide the relevant ethnomedicinal information, including the plant family, species, local name, portion utilized, and application.
TABLE 5: ETHNOMEDICINAL PLANTS USED FOR THE TREATMENT OF HEPATOBILIARY DISEASE IN ARUNACHAL PRADESH 39
| Scientific name | Family | Local name | Uses |
| Emblica officinales L. | Euphorbiaceae | Amla (P) | Fresh and dried fruits are used to treat liver disease, diabetes, and jaundice |
| Oroxylum indicum (L) Vent. | Bignoniaceae | Orok Tak Shein | Used in liver problem |
| Emblica
officinalis Gaertn |
Euphorbiaceae | Amolodi(Ap)
|
Fruits are used fresh as a liver tonic. The chewed dried fruits are used to treat diabetes, jaundice |
| Andrographis paniculata
(Burm.f.) Wall. ex |
Acanthaceae | Chiraitateeth(N) | The entire plant's extract is used for liver tonic and jaundice |
| Scoparia dulcis Linn. | Scrophulariaceae | Uykabnam | Used in Jaundice |
TABLE 6: ETHNOMEDICINAL USED FOR THE TREATMENT OF HEPATOBILIARY DISEASE IN ASSAM AND MANIPUR 41
| Scientific name | Local name | Family | Uses | |
| Assamese | Manipur | |||
| Aegle marmelos Linn | Bel | Heirikhagok | Rutaceae | diarrhea, Jaundice, diarrhea |
| Alstonia scholaris( L.) R.Br. | Satina | Barap lei | Apocynaceae | Ulcers |
| Artocarpus integrifolia | Kothal | Theibong | Artocarpaceae | diabetes, jaundice |
| Benincasa hispida (Thunb.) Cogn | Komora | Torbot | Cucurbitaceae | peptic ulcer, |
| Swertia chirayita (Roxb.exFleming) Karst. | Chirata | Chiretta | Gentianaceae | Liver disorder |
| Leucas aspera (WILLD.) SPRENG | Doron | Mayanglambum | Lamiaceae | Liver ailment |
| Ficus hispida L. Ficus glomerata Roxb. | KhohotaDimoru
|
Asi heibong
Heibong |
Moraceae
Moraceae |
liver ailments
Liver disorder |
| Jatropha curcus L. | Bongali era | awa-kege | Euphorbiaceae | Ulcer and jaundice |
| Nelumbo nucifera Gaertn.
|
Padum
|
Thambal
|
Nymphacaceae
|
Diarrhea, cholera, liver, cardiac complaints, and diabetes |
| Tinospora cordifolia Miers | Amoralota | ningthoukhongli | Menispermaceae | jaundice thirst vomiting |
TABLE 7: ETHNOMEDICINAL USED FOR THE TREATMENT OF HEPATOBILIARY DISEASES IN NAGAL-AND 42
| Scientific name | Family | Local Name | Uses |
| Ecliptaprostrata Roxb. | Asteraceae | Bhringaraja | Liver disorder |
| Averrhoa carambola L. | Oxalidaceae | Carambola | Jaundice |
| Boerhaviadiffusa L | Nyctaginaceae | Punarnava | Jaundice, spleen |
| Cassia fistula L. | Fabaceae | Aragvadha | Liver disease |
| Cuscuta reflexa Roxb. | Convolvulaceae | Amarbel | Liver disorder |
TABLE 8: ETHNOMEDICINAL USED FOR THE TREATMENT OF HEPATOBILIARY DISEASES IN MIZORAM 40
| Scientific Name | Family | Local Name | Uses |
| Dendrocnida sinuate | Urticaceae | Thakpui | For the treatment of jaundice, the root is cooked with crabs and the water is consumed. |
| Cinnamomum obtusifolia (BuchHam.) Sweet | Lauraceae | Thakthingsuak | The bark is used to treat liver issues and indigestion |
| Ficus semicordata Buch-Ham. Var. conglomerata (Roxb.) | Moraceae | Thenpui | Liver ailment |
| Scopariadulcis Medic | Scrophulariaceae | Perhpawng-chaw/ Hlothlum | To treat jaundice, the entire plant is crushed, and the juice is consumed. |
| Dillenia indica L. | Dilleniaceae | Kawrthindeng | For the treatment of jaundice, the fruit is boiled and water is ingested |
TABLE 9: ETHNOMEDICINAL USED FOR THE TREATMENT OF HEPATOBILIARY DISEASES IN MEGHALAYA 37
| Scientific Name | Family | Local name | Uses |
| Enhydra fluctuans Lour | Asteraceae | Kynbathingcha | The liver condition is treated with juice |
| Mimosa Pudica L. | Mimosaceae | Kynbatsamthiah | For the treatment of liver illness, a leaf infusion is consumed |
| Momordica charantia L. | Cucurbitaceae | Karela | Fruit juice is taken orally in the treatment of liver disease |
| Boerhaavia diffusa L. | Nyctaginaceae | Dieng puran | Leaf juice is taken for the treatment of jaundice |
| Hyplianthera stricta W. | Rubiaceae | Dieng diki | A leaf infusion is taken orally in the treatment of liver disease |
TABLE 10: ETHNOMEDICINAL USED FOR THE TREATMENT OF HEPATOBILIARY DISEASES IN TRIPURA 38, 44
| Scientific name | Family | Local name | Uses |
| Alocasia indica (Roxb.) Schott. | Araceae | Kochu, Muitu | Tuber is boiled and taken as food for the treatment of jaundice |
| Enhydra fluctuants Lour. | Asteraceae | Helencha | Boiled leaf for the treatment of jaundice |
| Hyptissuaveolens | Saururaceae | Tukma | Liver troubles |
| Moringa oleifera Lam | Rubiaceae | Sajna | Jaundice |
| Oroxylum indicum | Bignoniaceae | Nauka gas | Jaundice |
TABLE 11: ETHNOMEDICINAL USED FOR THE TREATMENT OF HEPATOBILIARY DISEASES IN SIKKIM 43
| Scientific Name | Family | Local Name | Uses |
| Podophyllum hexandrum | Berberidaceae | Bankankari | Used for jaundice, liver disorders, |
| Swertia chiraita | Gentianaceae | Chiraita | Used for liver disorders |
| Aesandrabutyraceae | Sapotaceae | Chewri | Used for liver protection |
| AbrusPrecatorius | Fabaceae | Lalgeri | Roots used for jaundice |
| Terminalia ballerica | Combretaceae | Barra | Used in Hepatitis |
DISCUSSION: With the use of that information, investigators were able to make rudimentary Phyto-medicinal extracts that could be used to treat a range of ailments, from simple ones like the common cold to more complicated ones like diabetes and cancer. These traditional herbal remedies nearly often involve traditional rites, rituals, and beliefs. Medical medicines are frequently always consecrated using prehistoric beliefs and rituals before being provided for the treatment of various Hepatobiliary illnesses. The current review's findings verified and confirmed prior studies' results that traditional local healers had a thorough understanding of how to use different plant parts and medicinal plants for a variety of illnesses and disease types.
As an ethnomedical remedy, our investigation unquestionably demonstrates the significance of Piper beetle plants to the household environments of these two societies. This species' high ethnomedicinal status may be explained by the Areca nut and the fact that it is consumed almost every day as part of their cultural practices. The ethical resides of these sites appear to come up short on information, awareness, and ethnomedicinal capacities fundamental for treating pneumonic diseases, despite informants mentioning many plants throughout this disquisition.
This may be the result of the fact that neither of these two villages' residents suffers from lung-related diseases regularly. We hypothesize that these fundus alterations are caused by hyperammonemia, hypo-albumin anemia, and reduced estrogen release; these are all pathological indicators of severe liver diseases and indicators of weakened liver function. Hepatic retinopathy is known to result from acute hyperammonemia-induced damage to Muller cells. Because hypoalbuminemia lowers oncotic pressure and increases intravenous hydrostatic pressure, it may encourage the plasma extravasation components and the development of retinal exudates. Hormonal alterations caused by high estrogen may result in retinopathy. Fundus images may demonstrate how blood cell sequestrations in splenomegaly result in anemia and blood cell apoptosis, notably, the fundus model and slit-lamp model additionally showed some identification of less severe hepatobiliary ailments, such as chronic viral hepatitis, non-alcoholic fatty liver disease, gallstones, and liver cysts. Showing the presence of morphological changes that have not been reported by earlier studies investigating liver diseasesshowing the presence of morphological abnormalities that haven't been discussed in past research looking into hepatobiliary illnesses.
CONCLUSION: The present study's findings might further focus on the value of historically used medicinal plants for various ailments. The bulk of the discovered plants has at least a few notable medicinal properties that align with most conventional ideas.
It may also be helpful in upcoming pharmaceutical and medical research efforts that might lead to breakthroughs to draw on this ancient knowledge of using plants to treat a range of illnesses and problems. Additionally, study into traditional knowledge and practices may help save rapidly vanishing regional knowledge, traditions, and medicinal plants so that they will be preserved for use by future generations.
ACKNOWLEDGEMENT: I thank the Department of Pharmaceutical Technology, University of North Bengal, and respective seniors and friends for their expertise and assistance throughout all aspects of our study and for their help in writing the manuscript.
REFERENCES:
- Muneeb A, Ahmad I, Ahmad MSA, Fatima S, Hameed M, Ahmad F & Hassan IFZ: “Ethnobotanical and economic uses of some medicinal plants from native saline areas”. International Journal of Applied and Experimental Biology 2023; 2: 2. doi: https://eminentscientists.com/.
- Siram J, Hegde N, Singh R and Sahoo UK: “Cross-cultural studies of important ethnomedi-cinal plants among four ethnic groups of Arunachal Pradesh, Northeast India,” Ethnobotany Re-search and Applications 2023; 25: doi: 10.32859/era.25.12.1-23.
- Tamang S, Singh A, Bussmann RW, Shukla V and Nautiyal MC: “Ethno-medicinal plants of tribal people: A case study in Pakyong subdivision of East Sikkim, India,” Acta Ecologica Sinica 2023; 43(1): 34–46. doi: 10.1016/j.chnaes.2021.08.013.
- Chandra S: “Folk Healing Practices of the North-East States,” 2023; 111–131. doi: 10.1007/978-981-19-4286-07.
- Aftab F, Qureshi R, Munnawar T, Waheed A, Rashid M, and Rehman S: “Quantitative analysis of ethnomedicinal plants of Tehsil Khuiratta, Azad Jammu & Kashmir, Pakistan,” Ethnobotany Research and Applications 2023; 25. doi: 10.32859/era.25.37.1-28.
- Das RJ: “Clerodendrum colebrookianum Walp: An Insight into its Pharmacology, Expository Traditional Uses and Extensive Phytochemistry. Current Traditional Medicine 2022; 9: 2. doi: 10.2174/2215083808666220623112606.
- Dunoma A, Ajibade GA and Moltong Yilwa V: “Eastern Journal of Agricultural and Biological Sciences (EJABS) Ethnobotanical Survey of Medicinal Plants in Seven Local Gov-ernment Areas of Zone A, Yobe State, Nigeria”, [Online]. Available: https://qabasjournals.com/index.php/ejabs
- Fu X, Chen S, Xian S, Wu Q, Shi J and Zhou S: “Dendrobium and its active ingredients: Emerging role in liver protection,” Biomedicine & Pharmacotherapy 2023; 157: 114043, Jan. doi: 10.1016/j.biopha.2022.114043.
- Neog PR and Konwar BK: “The distribution, economic aspects, nutritional, and therapeutic potential of swamp eel Monopteruscuchia: A review,” Fish Res 2023; 261: 10663. doi: 10.1016/j.fishres.2023.106635.
- Angupale JR, Tusiimire J and Ngwuluka NC: “A review of efficacy and safety of Ugandan anti-malarial plants with application of RITAM score. Malar J 2023; 22(1): 97. doi: 10.1186/s12936-023-04486-6.
- Hein PP, Arunachalam K, Fu Y, Zaw M, Yang Y and Yang X: “Diversity of medicinal plants and their therapeutic usages of Kachin people (Jinghpaw) in the central part of Kachin State, Myanmar,” J Ethnopharmacol 2023; 302: 115921, Feb. doi: 10.1016/j.jep.2022.115921.
- Mincheva I: “Ethnobotanical and Ethnopharmacological Study in the Bulgarian Mountain Rhodopes: Part II—Contemporary Use of Medicinal Plants. Diversity (Basel), 2023; 15(4): 482. doi: 10.3390/d15040482.
- Pasdaran A: “Some European Gentiana Species Are Used Traditionally to Cure Wounds: Bioactivity and Conservation Issues,” Diversity (Basel) 2023; 15(3): 467. doi: 10.3390/d15030467.
- Ansari T, Saleem M, Asif M, Prasad SB, Kumar V and Meena R: “Morphological, phytochemical and ethnopharmacological attributes of Xylosma longifolia Clos: A review. J Pharmacogn Phytochem 2023; 12(1): 679–689. doi: 10.22271/phyto.2023.v12.i1f.14613.
- Dissanayake I: “Taxus wallichiana: The Himalayan Yew,” in Immunity Boosting Medicinal Plants of the Western Himalayas, Singapore: Springer Nature Singapore 2023; 541–559. doi: 10.1007/978-981-19-9501-9_22.
- Reddy S: “Revival of Local Health Traditions from Healers Perspectives: Urgency of Recogni-tion and State Support 2023; 347–368. doi: 10.1007/978-981-19-4286-0_22.
- Gaobotse G: “The use of African medicinal plants in cancer management,” Front Pharma-col 2023; 14: doi: 10.3389/fphar.2023.1122388.
- Parashar S, Gautam RK, Goyal R, Sharma S, Gupta S and Mittal P: “An Insight View on the Role of Herbal Medicines in Infectious Diseases. Current Traditional Medicine 2023; 9(4): doi: 10.2174/2215083808666221006120944.
- Kalita A: “Arisaema Jacquemontii Blume, Jacquemont’s Cobra Lily,” in Immunity Boosting Medicinal Plants of the Western Himalayas, Singapore: Springer Nature Singapore 2023; 59–76. doi: 10.1007/978-981-19-9501-9_3.
- Wiegand J and Berg T: “The etiology, diagnosis and prevention of liver cirrhosis: part 1 of a series on liver cirrhosis. Dtsch Arztebl Int 2013; 110(6): 85–91. doi: 10.3238/arztebl.2013.0085.
- Wang R, Tang R, Li B, Ma X, Schnabl B and Tilg H: “Gut microbiome, liver immunology, and liver diseases,” Cell Mol Immunol 2021; 18(1): 4–17. doi: 10.1038/s41423-020-00592-6.
- Loomba R, Friedman SL and Shulman GI: “Mechanisms and disease consequences of nonalcoholic fatty liver disease. Cell Elsevier B V 2021; 184(10): 2537–2564. doi: 10.1016/j.cell.2021.04.015.
- Mitra S, De A and Chowdhury A: “Epidemiology of non-alcoholic and alcoholic fatty liver diseases. Transl Gastroenterol Hepatol 2020; 5: 16, doi: 10.21037/tgh.2019.09.08.
- Chakrabartty I and Rangan L: “Alpinia nigra and Its Bioactive Compound, Labdane Diterpene: A Review of Their Phytochemical and Biopharmaceutical Potential,” in Conservation of Biodi-versity in the North Eastern States of India, Singapore: Springer Nature Singapore 2023; 227–248. doi: 10.1007/978-981-99-0945-2_13.
- Iwakiri Y and Trebicka J: “Portal hypertension in cirrhosis: Pathophysiological mechanisms and therapy,” JHEP Reports 2021; 3(4): 100316, Aug. doi: 10.1016/j.jhepr.2021.100316.
- Fazliddinonvna G, Adkhambek M and Nurboboyev U: “Treatment of Mechanical Jaundice via the Modern Way. 2021; 2: [Online]. Available: www.scientificprogress.uz
- Ginko E, Alajmovic Demirović E and Šarić-Kundalić B: “Ethnobotanical study of traditionally used plants in the municipality of Zavidovići, BiH,” J Ethnopharmacol 2023; 302: 115888 doi: 10.1016/j.jep.2022.115888.
- Rawla P, Sunkara T, Thandra KC and Barsouk A: “Epidemiology of gallbladder cancer. Clin Exp Hepatol 2019; 5(2): 93–102, doi: 10.5114/ceh.2019.85166.
- Khouchlaa A: “Traditional Uses, Bioactive Compounds, and Pharmacological Investigations of Calendula arvensis: A Comprehensive Review. Adv Pharmacol Pharm Sci 2023; 1–27: 2023, doi: 10.1155/2023/2482544.
- Arroyo V, Moreau R and Jalan R: “Acute-on-Chronic Liver Failure,” New England Journal of Medicine 2020; 382(22): 2137–2145. doi: 10.1056/NEJMra1914900.
- Gillessen A and HHJ: Schmidt, “Silymarin as Supportive Treatment in Liver Diseases: A Narrative Review,” Adv Ther 2020; 37(4): 1279–1301. doi: 10.1007/s12325-020-01251-y.
- Rajaratnam M, Prystupa A, Lachowska-Kotowska P, Załuska W and Filip R: “Herbal medicine for treatment and prevention of liver diseases. Journal of Pre-Clinical and Clinical Research 2014; 8(2): 55–60. doi: 10.5604/18982395.1135650.
- Kumar Y and Sahoo G: “Prediction of different types of liver diseases using rule based classification model,” Technology and Health Care 2013; 21(5): 417–432. doi: 10.3233/THC-130742.
- Li X: “Investigation of herbal plant medicines Baishouwu on the mechanism of the digestion of body: A review,” J Funct Foods 2023; 100: 105379. doi: 10.1016/j.jff.2022.105379.
- Deka K and Nath N: “Traditional Hepatoprotective Herbal Medicine of Bongaigaon District, Assam (N.E. India),” American Journal of Ethnomedicine 2015; 2(5): [Online]. Availa-ble: www.ajethno.comhttp://www.ajethno.com
- Mohd Salim J, Anuar SN, Omar K, Tengku Mohamad TR and Sanusi NA: “The Impacts of Traditional Ecological Knowledge towards Indigenous Peoples: A Systematic Literature Review Sustainability 2023; 15(1): 824. doi: 10.3390/su15010824.
- Dolui AK, Sharma HK, Marein TB and Lalhriatpuii T: “Folk herbal remedies from Meghalaya 2004.
- Choudhury PR, Choudhury MD, Ningthoujam SS, Das D, Nath D and Talukdar AD: Ethnomedicinal plants used by traditional healers of North Tripura district, Tripura, North East India. J Ethnopharmacol 2015; 166: 135–148. doi: 10.1016/j.jep.2015.03.026.
- Khongsai & Kayang P: “Ethnomedicinal plants used by different tribes of Arunachal Pradesh 2011.
- Rai PK and Lalramnghinglova H: “Ethnomedicinal Plant Resources of Mizoram, India: Implication of Traditional Knowledge in Health Care System 2010.
- Hazarika R, Abujam SS and Neog B: “Ethno Medicinal Studies of Common Plants of Assam and Manipur Molecular Characterization of Genetic diversity of wild and cultivated varie-ties of Garcinia in Assam View project 2012. [Online]. Available: https://www.researchgate.net/publication/267962249
- Shankar R, Tripathi KA and Kumar A: “Conservation of some pharma-ceutically important medicinal plants from dimapur district of nagaland,” 2014. [Online]. Available: www.wjpr.net
- Chettri U and Kumari S: A list of medicinally important plants of Sikkim Himalayan region, India. Journal of Medicinal Plants Studies 2021; 9(4): 24–27.
- Sen S, Chakraborty R, De B and Devanna N: “An ethnobotanical survey of medicinal plants used by ethnic people in West and South district of Tripura, India. J for Res (Harbin) 2011; 22(3): 417.
How to cite this article:
Das J and Sarkar BR: A review of ethnomedicinal plants and their traditional uses for the treatment of hepatobiliary disease by different tribes of North-east India. Int J Pharmacognosy 2023; 10(6): 284-98. doi link: http://dx.doi.org/10.13040/IJPSR.0975-8232.IJP.10(6).284-98.
This Journal licensed under a Creative Commons Attribution-Non-commercial-Share Alike 3.0 Unported License.
Article Information
1
284-298
1067 KB
928
English
IJP
Jyotirmoy Das * and Bapi Ray Sarkar
Department of Pharmaceutical Technology, University of North Bengal, Darjeeling, West Bengal, India.
jyotirmoydasnbu@gmail.com
07 June 2023
28 June 2023
29 June 2023
10.13040/IJPSR.0975-8232.IJP.10(6).284-98
30 June 2023